Story
Ms. D is a 26 year old nulliparous female who came to our clinic in May 2017 for treatment because she was experiencing burning pain with penetrative intercourse. She reports that her symptoms began a few months prior when she and her partner first attempted intercourse. She states that they tried a few times but she continued to experience the same symptoms.
Ms. D reports that she generally has had no discomfort with tampon use unless she is “in a rush” or “more tense than usual”; in these cases she reports that she would have difficulty with insertion and would opt to use a menstrual pad instead.
Ms. D reports that she has had some stress urinary incontinence since 2012 whenever she has ”a big, unexpected” sneeze. She states that she has had many “glute strains” and was treated for thoracic outlet syndrome as a teenager, though she does not recall which side. She recalls that, at some point growing up, she was told that she has a rotation in her spine (she does not remember which health care professional told her this), and that he/she attributed it the position she is in when playing hockey, which she has played since the age of 13.
Ms. D reports that she has had a significant decline in her vision starting two years ago. She recalls that her posture got quite bad around this time, as she had to move her eyes close to the monitor when using the computer.
Ms. D reports that she had a small fracture in the left side of her jaw after having her wisdom teeth removed in November 2016. Treatment was immobilization of her jaw for five weeks, after which she developed tracking problems in her temporomandibular joint which have persisted to the present.
She also reports that squats have always been difficult. She states that she always feels off balance when she does them, and feels that her glutes are too tight to execute the movement correctly.
Currently she plays a variety of sports recreationally, runs, and goes to the gym.
Meaningful Complaint
Ms. D’s main complaint was burning pain with penetrative intercourse. She reports that she and her partner were able to achieve penetration, but it was too uncomfortable to continue.
She also reports, as an aside, that she finds squats difficult and feels that her glutes are too tight to squat properly.
Diane
Can you hypothesize on a mechanism that could explain her difficulty with squats, tight glutes and her pain with penetrative intercourse?
Trish
One possible reason for the difficulty with squats, tight glutes and dyspareunia would be that there is overactivity in the muscles of the pelvic floor. This was the hypothesis that I went into the objective part of the exam with, after hearing her history. When the muscles of the pelvic floor are overactive, the opening of the vagina is narrower and less compliant (because the levator ani muscles are unable to adequately relax) which can cause increased discomfort with intercourse. In addition, if the nerve endings on the wall of the vagina are sensitized (peripherally sensitized, in this case, rather than central sensitization), which can occur from increased compression on the nerves as they pass through overactive muscles or after any trauma to the vaginal wall, then anything coming into contact with the vaginal walls could provoke pain. This could then lead to guarding behaviour of the pelvic floor muscles, further contributing to muscle overactivity. Fascial connections between the levator ani and obturator internus allow for increased tension in the levator ani to contribute to increased tension in the obturator internus. Because the obturator internus inserts on the femur, tension from the pelvic floor can act as a vector of pull on the hip via the pelvic fascia and obturator internus. This can alter the alignment and biomechanics of the hip (difficulty with squats), which can then lead to reactivity of other muscles of the hip, which can be perceived by the patient as “tight hips” or “tight glutes”. Ms. D’s story, however, ended up going beyond the pelvis, as I quickly realized when doing the objective examination.
Cognitive Belief
Ms. D reports that she was aware of the potential to aggravate her symptoms by continuing to attempt penetrative intercourse and have the muscles get tighter and tighter as they try to “guard” or “protect” in response to pain. She states that she believes tight muscles may be a contributing factor, as she has had a history of glute strains and feels that her hips are very tight.
Ms. D reports that she has a supportive partner who is willing to do what he needs to do to help.
Ms. D reports no history of physical or emotional trauma.
Meaningful Tasks
Ms. D’s meaningful task was penetrative intercourse with her partner.
Screening Tasks
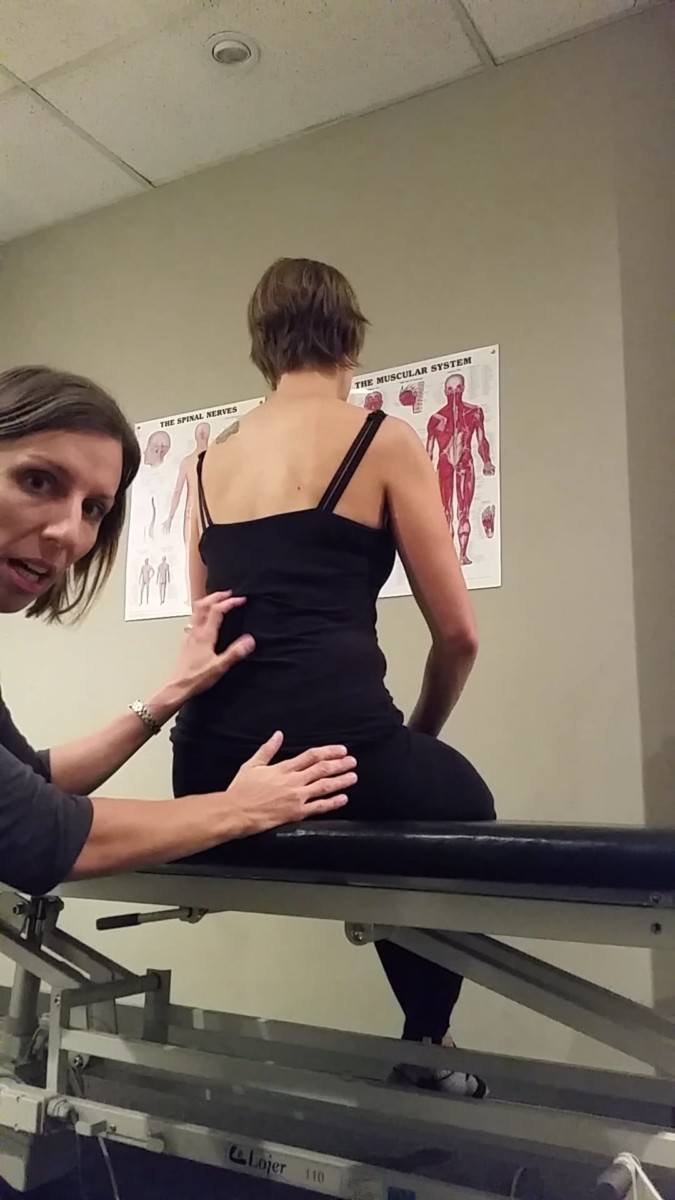
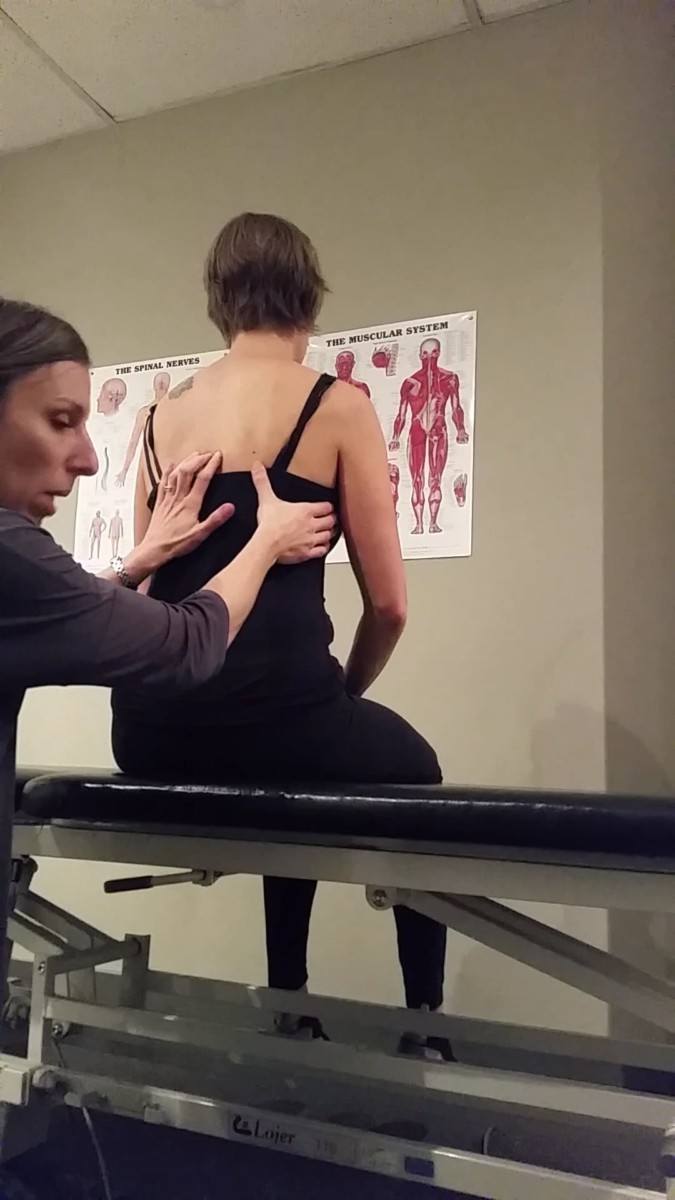
Standing Postural Screen
The standing position is used as a postural screen in the Integrated Systems Model to gain an understanding of where the individual’s body is in space, and to get a sense of any torsions, sways, or tilts there may be in their body in standing at rest. This is not to say that any of these are pathological, if they are found, as the patient may have no symptoms in static standing. It simply allows for observation of their alignment in standing. From here, one can make note of any changes from this starting position and determine if that change is an indication of sub-optimal or optimal biomechanics.
With her standing screen, it was noted that Ms. D had an intracranial (ICT) torsion to the right (her right temporal bone was posteriorly rotated, her left temporal bone was anteriorly rotated, and her sphenoid was rotated to the right), and C2 was rotated to the right and translated left. Visually, it appeared that her head was side flexed to the right. The 2nd and 3rd thoracic rings were translated to the right, rotated to the left, and below the 3rd ring the entire thorax was rotated to the left. The pelvis was in a left transverse plane rotation (TPR) and left intrapelvic torsion (IPT). Both femoral heads were translated anteriorly. In her first session, it was noted that there was a great deal of overactivity in the muscles of both hips (the glutes and the deep hip external rotators) such that precise palpation of the femoral heads was difficult.
Diane
An ICT pertains to the alignment of the left and right temporal bones and the occiput much like the two innominates and the sacrum in the pelvis. You note that the sphenoid was rotated to the right.
- Is this congruent or incongruent with the ICT?
- Was the position of C2 congruent with the ICT or incongruent.
- Was the cranium right sideflexed in relation to the neck?
- Given the biomechanics of the OA joints vs the cervical segments, which region would be more likely to cause this combination of findings?
- Were the 2nd and 3rd thoracic rings congruent, or incongruent to C2?
- Was the pelvis rotated congruent or incongruent to the 2nd and 3rd thoracic rings?
- What is the significance of determining regional congruence vs incongruence in the Integrated Systems Model?
- If both femoral heads were translated anteriorly, the net effect on the pelvis would be what?
Trish
Q1: If the cranium is in a right ICT and the sphenoid is rotated to the right, this is considered a congruent finding.
Q2: C2 rotated to the right is congruent with the right ICT. When the cranium moves into a right ICT there is a R side bending of the occiput (or a clockwise rotation along the coronal plane) which then induces a right rotation of the axis (C2) dictated by the attachments of the alar ligaments. It is the understanding of this anatomy and biomechanics that is the basis of the alar ligament stress test (Dvorak, Panjabi 1987).
Q3: The cranium was right sideflexed with respect the neck.
Q4: Normal coupling of the OA joints in the craniovertebral region is contralateral, such that the right sideflexion is coupled with left rotation. In the cervical spine, the coupling is ipsilateral such that right side flexion is coupled with right rotation. In Ms. D’s case, C2 was rotated right, sideflexed right, and translated left and the OA joint was side flexed right and rotated left (this may clarify a point you brought up later in the treatment section under the “align” heading). It was, therefore, the OA joints AND C2 that were contributing to the R side flexion.
Diane
There is an incongruence in the biomechanics reported here. You note that the ICT is to the right. This means that the right temporal bone is rotated posteriorly and the left temporal bone is rotated anteriorly and the occiput rotation in the transverse plane is to the right. This is inconsistent with your report that the OA joint was sideflexed right and rotated left – are you suggesting that the occiput was rotated to the left relative to the atlas or to the right relative to the atlas? Something seems off here! The cranium position may be driven by C2-3 or the AA joint and not the OA joint at all. I’m just trying to reconcile the biomechanics you’ve presented of the OA joint and the ICT! I agree that with a SCM vector that you note below the cranium as a unit would be right sideflexed and left rotated – it is the between occiput/atlas and axis/C2 position/biomechanics I’m trying to reconcile.
This question led to an in-depth review for both Trish and Diane of the osteo and arthrokinematics of the Occiput, atlas and axis, OA, AA and C2-3 joints in the scenario of her patient. With the following joint conclusion.
Trish
Yes, on reflection we agreed to the following; the OA joint is NOT contributing to the right side flexion/left rotation. If that was the case, the rotation of the occipital bone would have been incongruent to the temporal bones. In Ms. D’s case, there was a right ICT, with the sphenoid rotated to the right and the occiput rotated to the right in the transverse plane BUT the head and upper neck were right side flexed and left rotated in space. If the occiput right rotates in the transverse plane relative to the atlas, the biomechanics of the OA joint dictate that left sideflexion will also occur. Therefore, the AA joint is likely left rotated (to de-rotate the right rotation at the OA joint), and right sideflexed as a result of the pull from the right sternocleidomastoid.
So, in summary:
RICT: OA joint – occiput is rotated right and side flexed left relative to the atlas; right occipital condyle glides posteriorly, left occipital condyle glides anteriorly relative to the atlas (arthrokinematics)
C2-3 – C2 is rotated to the right and side flexed right, translated left; L C2 inferior facet glides superior-anterior-lateral, R C2 inferior facet glides inferior-medial-posterior
In between the OA joint and the C2-3 joints is the mobile adaptable AA joint.
AA joint – atlas rotates to the right in space and follows the right rotation of the occiput. C2 rotates further to the right than the atlas does and therefore relative to C2, the atlas is rotated left. This neutralizes the transverse plane rotation of the occiput and C2. The atlas is pulled into right side flexion right relative to C2 by the SCM vector. So at the joint level the AA joint is left rotated/right sideflexed. Arthrokinematics of the AA joint for this motion to occur: anterior glide on the right of C1 on C2, posterior glide on the left of C1 on C2. A different vector may result in a different combination of sideflexion/rotation at the AA joint.
With respect to congruencies, everything within the cranium was congruent (R ICT, R sphenoid, R occipital bone), and that was congruent with the direction of rotation of C2. The left rotation of C1, however, was incongruent to the C2 (C2 was rotated right, C1 was in a relative left rotation).
Contrary to what I stated above, however, it was not tension on the alar ligament that dictated the right rotation of C2 because the occipital bone was not side flexed right with respect to C1. It was sideflexed left and rotated right at the OA joint, which would slacken the left alar ligament, therefore the alar ligament would have no influence on the C2 rotation.
Diane
Takes an FCAMT level of biomechanical training combined with ISM training to work this out! Well done Trish.
Trish
Q5: The 2nd and 3rd thoracic rings were incongruent to C2 in that C2 was rotated right and translated left while thoracic rings 2 and 3 were rotated left and translated right.
Q6: The left transverse plane rotation of the pelvis was congruent to thoracic rings 2 and 3.
Q7: Noting areas of incongruence versus congruence is important in the Integrated Systems Model because it helps to guide you to areas that are not following the accepted biomechanics of the musculoskeletal system and may potentially be a driver for the task. One must consider congruence WITHIN a region and BETWEEN regions.
In terms of congruence BETWEEN regions, a finding is considered congruent if it is in a position that is in line with the biomechanics of the segments/joints above and below. In Ms. D’s case, the cranium and C2 were congruent because they were both rotating to the right. It was the left rotation of C1 relative to C2 that was incongruent. This area caught my attention as a potential area of interest.
Moving down from C2, there was a continuous rotation to the right, then when we got to the 2nd thoracic ring, the direction of rotation changed again; this was another area of incongruence.
Continuing caudally, the left transverse plane rotation of the pelvis was congruent to the left rotation/R lateral translation of the 2nd and 3rd thoracic rings because it followed the left rotation of the thorax below the 2nd and 3rd rings.
An example of incongruence WITHIN a region would be a left intrapelvic torsion and a right transverse plane rotation. A finding such as this would prompt you to look for two different vectors; one pulling the pelvis into a left intrapelvic torsion and one dictating the right transverse plane rotation.
Q8: If both femoral heads were equally anteriorly translated then there would be no net transverse plane rotation and there could be an anterior pelvic sway. However, if the anterior translation of one femoral head is greater than that of the other, then there would be a transverse plane rotation in the contralateral direction (ie: in the case of Ms. D, the right femoral head was anteriorly translated to a greater extent than the left, which resulted in a left transverse plane rotation).
Squat
A squat was chosen as the next screening task. Because of her reports of longstanding difficulty performing squats, as well as the fact that intercourse in a four point kneel position was one of the positions that they had tried and which had given her significant discomfort, it was important to determine if there was sub-optimal alignment, biomechanics and/or control around the pelvis and hip with moving into load-bearing hip flexion. If not, a better task may have been to have Ms. D go into a four point kneel position.
Diane
Absolutely – I’d go there right away since her feet are not loaded in 4 point kneeling but they are in a squat.
Trish
Yes, good point. At the time I chose a squat as she was quite far from even getting to 90 degrees of hip flexion so there were already multiple areas of failed load transfer by the time her hips were in enough flexion to accommodate a quadruped position. In hindsight, I could have had her in quadruped but had her hands on a table an increased the height of the table to accommodate the lack of hip flexion.
In Ms. D’s case; however, areas of sub-optimal alignment, biomechanics and control were immediately noted early in the squat task.
- The right sacroiliac joint (SIJ) lost control early in the squat, and it was noted that counternutation of the sacrum on the right side was the dominant movement, as opposed to an anterior rotation of the right innominate relative to the sacrum
- the left transverse plane rotation (TPR) of the pelvis increased, and both femoral heads remained anteriorly translated
- the right intracranial torsion increased early in the squat, and there was a strong pull into craniovertebral and upper cervical extension
- the 2nd and 3rd thoracic rings remained translated to the right/rotated to the left
Diane
A transverse plane rotation of the pelvis is commonly associated with a congruent intra-pelvic torsion. Why could Ms. D NOT have had an IPT in her squat task?
Trish
In Ms. D’s case there was a loss of control at her right SIJ and the sacrum moved into counternutation relative to the right innominate. In an IPT, the sacrum remains nutated relative to the right and left innominates. Therefore, by definition, she could not have had an IPT when she had a loss of control at the right SIJ.
A cranial correction (i.e.: unwinding the intracranial torsion) made a remarkable improvement in her squat task.
The alignment of C2 and the 2nd and 3rd thoracic rings automatically corrected with the cranial correction and remained corrected through the squat, and there was significantly less pull into upper cervical/craniovertebral extension (though this was not completely resolved). The right and left femoral heads remained anteriorly translated in standing but centered through the squat when the cranium was corrected, and Ms. D reported that they felt much freer than she can ever remember them feeling. There was less of a left transverse plane rotation of the pelvis and Ms. D was able to achieve a greater depth of squat prior to the sacrum moving into counternutation on the right.
The addition of a pelvic floor relaxation cue (imagine the sitz bones moving away from one another, the tailbone untucking, and the anal sphincter relaxing) further improved the alignment, biomechanics, and control at the pelvis with this task.
Given these findings, it was determined that the cranium was the primary driver and the pelvis was the secondary driver for the squat task.
Diane
What about the hips in standing? Did they center with this cue? They are not a driver for the squat task but didn’t change with the cranial correction in standing – did you try a cue in standing with the cranial correction?
Trish
I did not look at the addition of a pelvic floor relax cue to the cranial correction for the standing task because I felt that the squat and internal palpation were the screening tasks that related to the meaningful task. I used the standing screen as simply a screen to get a starting point for where her body is in space and then see how her alignment, biomechanics, and control changed from this position. For this reason, I was not concerned (at this point) that the femoral heads did not center in the acetabulum during standing. If her meaningful complaint involved performing a task in a standing posture, then I would have tried to find a combination of corrections that helped to bring the femoral head into the center of the acetabulum in standing. In this case, however, I made a note that the hips remained anteriorly translated in standing, and then moved on to finding the drivers for the squat and internal palpation.
Internal vaginal palpation in crook lying
When dyspareunia is the primary complaint, it is obviously not possible to reproduce the task in the clinic. However, a vaginal exam is typically performed as part of a pelvic health examination in order to assess muscle activity at rest, and the ability of the muscles to contract and relax, as well as to determine if there is any pain or hypersensitivity at the vaginal opening.
After obtaining consent from Ms. D, an internal vaginal exam was performed. With insertion of 2 gloved fingers to the distal interphalangeal joint, Ms. D reported 6/10 pain on the Numeric Pain Rating Scale. With self-correction of her cranium (which she had been taught prior to the vaginal exam) she reported that her pain immediately decreased to 2/10. Additional improvement was felt in muscle relaxation and Ms. D’s subjective report of pain decreased to 0/10 with pelvic floor relaxation cues. It was also noted that her right and left femoral head position improved, though there was still overactivity of the muscles of the hip so it was difficult to determine if this was a complete correction at the hips.
Given these findings, it was again determined that the cranium was the primary driver and the pelvis was the secondary driver.
Diane
And maybe the hips still required some treatment since they didn’t completely correct???
Trish
Yes, I kept thinking that the hips would probably require some treatment and, had I not been practicing in the model, I probably would have gone there first. But throughout the course of Ms. D’s treatment the hips never really presented themselves as strong drivers. Looking back at my notes, there were couple of sessions where we felt correction of a hip *may* have improved a task but they were surprisingly never really a focus of the treatment.
It is important to note that a pelvic floor relaxation cue alone was not sufficient to improve the squat task or to elicit a notable relaxation of the pelvic floor muscles and reported decreased pain at the vaginal opening. It was only with a cranial correction that the pelvic floor muscles were able to relax and the pain decreased.
Diane
Given her story, can you provide two different hypothesis as to how the pelvic floor muscles may react/respond to her primary cranial driver? What are two biologically plausible mechanisms.
Trish
Hypothesis 1 – Having the head and neck held in a position of right side flexion, with the addition of the incongruent left rotation and right lateral translation of rings 2 and 3, likely increased the tension on the dura. Anatomically, the physical connection of the dura to the pelvis is the filum terminale which is the distal extension of the meninges that attaches to the coccyx. Branches from the sacral plexus, which arises from S1-4, innervate the muscles of the pelvic floor (as well as the muscles of the hip) and, in response to the increased tension and decreased mobility of the nervous system, the muscles of the pelvic floor increased in activity in order to shorten and decrease tension on the system by decreasing tension through these sacral nerves. In this case, however, the increased activity of the muscles caused compression of the nerves passing through the pelvic floor muscles which contributed to the increased sensitivity of the nerve endings. In addition, increased pelvic floor muscle activity may have actually further increased tension and compression on the nerves of the sacral plexus. Branches of the sacral plexus supply the gluteal muscles (the superior and inferior gluteal nerves) as well as the deep muscles of the hips (nerves to piriformis, obturator internus, and quadratus femoris), and the feeling of increased tightness in her “glutes” may have been because irritation of these nerves caused overactivation of the muscles of the hips .
Hypothesis 2 – WIth the neck held in a position of right side flexion there was a right rotation and left lateral translation of C2 and an incongruent left rotation and right lateral translation of the 2nd and 3rd rings. It is possible that these rings shifts had been present for an extended period of time (recall in her history she has had a history of thoracic outlet syndrome, was told she had a “twist” in her spine, stick-handled on the right when she played hockey, has noticed postural changes since her eyesight began declining two years ago) which may have contributed to movement and postural strategies that caused an increase in thoracic and abdominal muscle activation. This may have contributed to increased intra-abdominal pressure which may have caused a downwards force on the abdominal and pelvic organs. This could have resulted in an increased resting activation of the muscles of the pelvic floor to provide support for the pelvic organs.
*Note* On her initial assessment I had felt that the 2nd and 3rd rings corrected with the cranial correction. However, in subsequent treatments I noted that the 2nd and 3rd rings were acting as a secondary driver and required some treatment. I think, in hindsight, that the ring shifts were so marked initially and improved significantly with the cranial correction that I didn’t pick up that it wasn’t a full correction. It was only at a later session when I was hunting for contributing secondary drivers that I noted that the 2nd and 3rd rings were still slightly translating right with the meaningful tasks. It was at that point that I used a dry needling technique to the local segmental muscles (see the Subsequent Sessions section). When thinking it through, it didn’t make sense that the 2nd and 3rd rings would have resolved fully with the cranial correction if they had been present for the length of time that her story suggests. Hence why they were still there and required treatment to further improve her symptoms.
Diane
Excellent reflection and hypothesis development for mechanisms!
Vector Analysis
Cranium
In order to determine the vectors of the primary driver for both tasks (the cranium) a passive listening technique was used, in which the right ICT was initially corrected and then slowly released as the therapist’s hands felt for the direction of pull.
The primary direction of pull was in the anterior part of the neck, obliquely down towards the manubrium. It was determined that this first vector that needed to be addressed involved the neural system, and the pull was the result of overactivation of the right sternocleidomastoid.
Once the right sternocleidomastoid was released with a Release With Awareness technique, there was an underlying short vector pulling anteriorly on the right mastoid process that was determined to be the posterior belly of the digastric. This was felt to be a myofascial as well as a neural system impairment. It is noted that the distal attachment point of the digastric is the mandible, via a tendinous arch on the hyoid which, one would expect, is more mobile than the cranium. Therefore the vector is unlikely to be the digastric alone, but additionally any of the myofascial tissue directly adjacent to it.
Diane
Can you describe the difference in the quality of the passive listening from a myofascial system vs neural system impairment?
Trish
When performing a vector analysis, a neural system vector will have an elastic quality to it. The correction can typically be made fairly easily, and then when the correction is released, there will be a slow pull along the direction of the vector, much like slowly releasing a spring. A region held by a myofascial vector will feel more difficult to correct, much like pulling on a piece of leather, and on release will be a firmer, faster pull in your hands.
Pelvis
Active joint mobility
The standing open kinetic chain hip flexion task was performed to assess the active joint mobility of the pelvis. With optimal active joint mobility, you would expect to see a posterior rotation of the innominate and relative nutation of the sacrum as the ipsilateral hip is brought into flexion, with no flexion through the lumbar spine. In the case of Ms. D, mobility of both the right and left sacroiliac joints were decreased in that as the hip was brought into flexion there was a posterior rotation of the entire pelvis and flexion of the lumbar spine. These non-optimal findings appeared to be symmetric when comparing the right and left sides.
Active control
In order to assess the active control of the sacroiliac joints, Ms. D was asked to come into a squat while the therapist palpated the sacrum and the right innominate. It was noted that the right sacroiliac joint lost control very early in the squat, and it was noted that there was a strong caudal pull drawing the sacrum into counternutation rather than a vector pulling the innominate into anterior rotation. The same depth of squat was repeated on the left side, and control of the left sacroiliac joint was maintained within this depth. At this point of the exam, active control of the left sacroiliac joint with a deeper squat was not assessed.
Note that a single leg stance could have been used to assess active control of the SIJs, but given that the squat task was also a meaningful task, a squat was used instead.
Passive joint mobility
Passive joint mobility focussed on the right SIJ, as this was the side where an earlier loss of control was noted. When assessing the neutral zone of the right SIJ in the superior, middle, and inferior parts, decreased mobility was noted in the middle and inferior part, indicating that the piriformis, ischiococcygeous, and levator ani were all contributing to decreased SIJ mobility. There was decreased mobility noted on the left, as well, but to a lesser degree than the right.
Passive control
Passive control was not tested at this time. The vectors crossing the sacroiliac joints were compressing the joints and were not allowing for the joints to be taken into their close packed position. Tests to assess the integrity of the ligaments could not be performed correctly and reliably without the vectors first being released.
Based on these findings, it was determined that there was a neural system impairment within the pelvis, specifically it was the muscles of the pelvic floor that were contributing to decreased mobility (bilateral) and control (right) of the sacroiliac joints.
Diane
What findings from Ms. D’s story suggest that an assessment of her dural/neural mobility is indicated?
Trish
Starting with the subjective history, I began to think that I may need to investigate Ms. D’s neuromobility. She reported a history of thoracic outlet syndrome, which may be related to decreased neuromobility, and states that she realized that she has what she called “a lot of neural tension” when studying in university. Clinically, I have commonly seen a pattern of increased pelvic floor muscles activity, overactive hips, and increased neural tension, and so I kept it in my head that this could potentially be part of the story for Ms. D. Once I found the connection between the cranium and the pelvic floor when I was looking for drivers, I determined that it would be necessary to see if there was a dural vector between them. Anatomically the dura connects from the cranium to the coccyx so I acknowledged that it was a possibility. However, as I proceeded with the exam, I noted that the cranial vector was extracranial rather than intracranial (ie: not dural) and the pelvic vector was within the pelvis. My next step, then, was to see if the position of the cranium and upper cervical spine and the tension in the pelvis was contributing to decreased neural mobility. I then proceeded with a straight leg raise and investigated how correcting the cranial and pelvic drivers changed the neural mobility.
Dural/neural mobility
During the internal palpation part of the objective exam, it was noted that there was increased tension in the nerves of the sacral plexus as they pass along the posterior aspect of the pelvis on the right and left sides. This, combined with the subjective history of past thoracic outlet syndrome and decreased neural mobility that was discovered when studying with colleagues, as well as the alignment of the hips and the decreased ability of the hips to move easily into flexion with a squat suggested that assessment of the dural/neural mobility was warranted. In addition, understanding the anatomy of the dura and its connections from the cranium to the coccyx suggested that it was important to assess the mobility of the nervous system to investigate the dura as being a possible vector for the between the cranium and the pelvis.
A straight leg raise was chosen in order to determine if lack of neural mobility could have been what was contributing to decreased hip flexion and the loss of control at the right SIJ. It would also give an idea if there was general decreased mobility of the nervous system. With a straight leg raise test, R1 (the beginning of resistance to the movement) came on at 60 degrees for the right hip and 45 degrees with the left hip. Both a cranial correction and a cue to relax the pelvic floor (alone and, to a greater degree, together) increased the range of motion before the onset of R1 with the straight leg raise test. Therefore it was determined that the nerves were not a vector, but rather the increased neural tension was the result of decreased mobility of the nerves in the “container”.
So, in conclusion, the vector for the pelvis was determined to be the pelvic floor muscles, as a unit rather than one or two specific bands of muscle, and this was considered to be a neural system impairment.
Diane
Awesome clinical testing and reasoning. The other thing I’ve been doing lately is adding a pelvic floor contraction and release which holding the cranium corrected before I add any peripheral leg or arm movements. My belief is that we should be able to contract our pelvic floor muscles and not feel any pulling on the cranium. A similar experience should be felt with pelvic floor muscle relaxation. If activation or relaxation of the PFM causes tension, tugs, pulls on the cranium, then there is still release to be done in the spinal canal/coccyx region before moving onto the extremities.
Summary of findings
In summary, Ms. D’s meaningful task was penetrative intercourse with her partner, and the screening tasks were a squat and internal vaginal palpation (which is a standard part of a pelvic floor assessment). From the assessment, it was determined that the primary driver for both tasks was the cranium and the secondary driver was the pelvis. The first detected vector for the cranium was the right sternocleidomastoid (neural system), and then the posterior belly of the digastric was noted (neural and myofascial). The pelvic vectors were the ischiococcygeous and iliococcygeous, with the pubococcygeous and puborectalis contributing to a lesser degree.
Given these findings, it was hypothesized that the intracranial torsion and the overactivity of the pelvic floor muscles were contributing to decreased mobility in the nervous system. This decreased neural mobility was preventing pure flexion at the hip joint with the squat task, and the increased tension in the nervous system was leading to hypersensitivity of the nerve endings at the introitus.
Diane
But you weren’t sure if the hips were still involved?
Trish
At this point I still suspected that the hips may need some treatment in subsequent sessions. I expected that there would be some improvement with treatment of the cranium and relaxation of the pelvic floor but suspected that I would be hunting around for other secondaries and that the hips would be it. But surprisingly they required little treatment. As I stated earlier in response to your comment about the hips, I did a little bit of release work around the hips, but they never seemed to present as a primary or strong secondary driver. As we worked on everything else, specifically the movement piece to her treatment, the hips seemed to “sort themselves out”.
Diane
Very cool. We can have the best ‘left-brained treatment plan and hypothesis’; however, the beauty of ISM is that the patient and their experience lets you know ‘what’s next’ and when.
Initial treatment session
Release
The first vector that was targeted was the right sternocleidomastoid muscle. A Release With Awareness technique was used, in that the muscle was held in a shortened position until it was felt to soften while cues were giving to visualize the muscle lengthening/relaxing, then it was taken into a stretch.
Diane
Describe the neurophysiological mechanism by which shortening a muscle reduces its neural drive.
Trish
Within the belly of a muscle are groups of intrafusal muscle fibers called muscle spindles. Afferent nerve fibers wrap around these muscle spindles and detect changes in length of the muscle. When there is a stretch on the muscle spindle (such as when there is tension on the muscle because it is held in a non-optimal position), this message is carried to the spinal cord by the afferent fibers. After synapsing in the spinal cord, a signal is then sent along the efferent alpha motor neuron to the extrafusal muscle fibers and elicits a contraction which presents clinically as an overactive muscle fascicle or fascicles. When using a release with awareness technique, the shortening of a muscle, either by changing the position of the joint the muscle crosses or approximating two points of the overactive muscle, shortens the muscle spindle within the muscle which alters the afferent input being sent to the spinal cord. Because the stretch of the muscle is no longer being detected by the afferent fibers there is a decrease in the signal being sent along the efferent motor neuron resulting in a relaxation of the muscle fibers. The addition of cues to “soften”, “relax”, “lengthen” make use of the motor cortex’s influence in motor control, adding inhibitory signals from the higher order descending pathways.
Diane
Apparently, (and I just learned this a couple months ago but can’t remember where I read this!) the muscle spindle is not in the muscle fibre but in the connective tissue within the muscle i.e. now thought to be a fascial receptor.
Once the sternocleidomastoid was released, the posterior belly of the digastric was determined to be the vector of pull. A Release With Awareness technique was used, then the remaining myofascial restriction was resolved with myofascial release.
In the first session, there was such a dramatic improvement in the tasks with cranial correction that the focus was on releasing the vectors of the cranium. No manual release work was performed on the pelvic floor muscles. Instead, Ms. D was taught how to recognize tension in her pelvic floor and how to use her breath and visualization to relax the pelvic floor muscles. She was encouraged to visualize the pelvic floor moving in a coordinated fashion with her diaphragm and, when she inhaled, to picture her diaphragm descending and her pelvic floor softening and descending as well.
To address the tension in her cervical musculature, she was encouraged to also visualize her neck and throat softening and relaxing as she worked on the breathing and visualization for the pelvic floor. She was encouraged to start focussing on one area at a time then, as she became more comfortable, work on relaxing both the neck and pelvic floor together.
Align
For her align cues, Ms. D stood in front of a mirror and observed her tendency to hold her head in right side flexion and slight left rotation. She was cued to use the position of her eyes to correct the way she holds her head, and it was explained to her the importance of using her vision to retrain her head and neck posture as her kinesthetic awareness of her head in space was altered from years of holding it in right side flexion. The anatomy of the sternocleidomastoid was reviewed, and she was instructed to visualize lengthening of this muscle to allow for the corrected neck position.
Connect
Once the cranial vectors were released, Ms. D was able to correct the alignment of her cranium and upper cervical spine, although she was not able to maintain this position when her attention was taken away from it due to dysfunction of the motor control of the deep cervical musculature. For this reason, Ms. D was instructed in deep neck flexor retraining exercises.
Diane
In the ISM approach, motor control training for the deep segmental muscles is determined by assessing the response of segment control with drivers corrected. Ms. D was able to correct and maintain alignment of her neck and upper cervical spine with her cranial correction. How would training the deep neck flexors help her maintain the alignment of her cranium – the piece that you determined to be essential for postural control of her neck?
Trish
Ms. D’s motor control issue was a two-part problem. Yes, the deep neck flexors were able to help control the cervical spine when the cranium was corrected, but she lacked endurance of the muscles and kinesthetic awareness. She was able to briefly maintain alignment of her neck after the cranial vectors were released but could not sustain this, especially if her attention was diverted or if she was unable to look in the mirror when finding the corrected alignment of the neck and cranium. This could have been from lack of endurance of the deep neck flexor musculature, as well as from a lack of awareness of joint position from (possibly) years of sub-optimal alignment and biomechanics. The purpose of the deep neck flexor exercises was to increase the endurance of the deep neck flexors as well as improve her kinesthetic awareness and proprioception of the upper cervical spine.
Diane
Now called Stage 2 capacity training for the optimal strategy!
Move
Ms. D was encouraged to focus on the alignment of her neck/cranium and relaxation of the pelvic floor when standing, moving into a sitting position, and having intercourse (she was encouraged to try if she felt comfortable doing so).
Further structured movement exercises were saved for subsequent sessions.
Followup treatment sessions
Ms. D was seen once per week for treatment.
After her initial treatment session, Ms. D reported that she was finding it much easier to hold her head in a neutral position, and the range of motion of her squats was much improved. She was able to involve her partner in internal release techniques of the pelvic floor. She also reported that the tracking of her jaw felt like it had improved with the cranial work.
Diane
Describe biomechanically how tracking of the TMJ would improve specifically with a right ICT?
Trish
Optimal biomechanics for opening of the TMJ are described as follows: The mandibular condyle anteriorly slides and posteriorly rolls on the disc within the glenoid fossa of the temporal bone in the first phase of opening. Then the condyle and disc translate antero-inferiorly down the articular eminence of the temporal bone. Then, in order to achieve maximal opening, there is an additional anterior slide and posterior roll of the condyle while the position of the disc remains unchanged. In the case of an intracranial torsion (ICT) there would be an altered “starting position” of the right and left mandibular condyles. With a right ICT, the posterior rotation of the right temporal bone would cause a relative anterior rotation of the right side of the mandible (jaw opening) or posterior roll of the condyle within the fossa. The opposite would be true of the left TMJ. Therefore, when the patient would open her mouth, the left side would have to “catch up” to the right, which could be interpreted as a problem with the tracking of the jaw. In the case of Ms. D, we must also consider that the myofascial tension coming from the area under her right mastoid process, specifically the posterior belly of the digastric, would alter the tracking of her jaw. Given the attachments of the digastric (from the mastoid process to the mandible via the hyoid), one could consider that myofascial tension in this area would further contribute to the asymmetry of the starting position of the condyles.
The focus of her first four treatment sessions had been on cranial/cervical release work, external release of the pelvic floor, neural mobility exercises, and breath work and visualization to relax the pelvic floor. It was not until her fifth treatment session that we did any internal release work for the pelvic floor.
After her fourth session, Ms. D reported that she had been able to have penetrative intercourse. She reported that there was initially pain with penetration, but as she focused on relaxation of the pelvic floor she was able to continue and reported that pain was 0/10. She did note that this was in the supine position, and that there was still discomfort in quadruped.
Over the course of her treatment sessions, Ms. D reported that squats became much easier and she was able to squat much deeper without the feeling of tension in her glutes. Objectively, it was noted that the range of motion of her squat significantly increased, with the femoral heads remaining centered in the acetabulum and the sacrum nutated. She reported that she was consistently able to hold her head in a neutral position, though she still felt tension in the neck musculature on occasion. Throughout her treatment, Ms. D reported occasional symptoms of increased neural tension in her arms (tension in the forearms and paresthesias) after increased charting at work or excessive lifting. This was determined to be partially cranially driven, and was addressed with treatment to the cranium and local muscle release.
Because squats were no longer useful as a screening task, we changed the screening task to rocking back in a quadruped position. Recall that it was stated previously that this was the next reasonable progression given Ms. D’s meaningful task. In addition to the cranial primary driver, it was noted that correction of the clavicles allowed for increased range of motion in this quadruped position. The vector for this secondary driver was determined to be the clavicular fibers of pectoralis major, which were treated with a release with awareness technique, postural education, and independent stretching and mobility exercises.
Additionally, local segmental muscle (multifidus and rotatores) hypertonus was found at T1-2 and T2-3 to be contributing to the right translation of thoracic rings 2 and 3. Once these local vectors were treated with a dry needling technique, the remaining restrictions to neural mobility improved and Ms. D’s lingering symptoms decreased to the point that she was discharged from treatment with encouragement to continue with her homework as needed and follow-up if her symptoms returned.
Diane
Awesome case report Trish!
Skills Demonstration
Diane
In order to be conclusive that the 6th thoracic ring was the best correction, Trish should have had the patient do a co-correction of the 2nd and 3rd thoracic rings (which improved the shoulder girdle) while she corrected the 6th thoracic ring to see if the upper thorax was a contributor. She didn’t specifically tell us which cervical segments were left rotated – those should have been checked in the neck right rotation task and corrected as well. The ICT correction looked like it made the task worse, I’d be interested in knowing the relationship between C2 and the ICT and C7 and the 2nd thoracic ring. Why do combined corrections when one area makes a bigger difference than the others? A residual driver (secondary) can ‘bring the entire pattern’ back between sessions and spending a bit of time on both areas seems to result in longer lasting change.
Message: Don’t stop at the first correction that improves the task! A habit we all fall victim to at times.
Case Study Author
Clinical Mentorship in the Integrated Systems Model
Join Diane, and her team of highly skilled assistants, on this mentorship journey and immerse yourself in a series of education opportunities that will improve your clinical efficacy for treating the whole person using the updated Integrated Systems Model.
We will come together for 3 sessions of 4 (4.5) days over a period of 6-8 months with lots of practical/clinical time to focus on acquiring the skills and clinical reasoning to put the ISM model into practice. Hours of online lecture and reading material and 12 hours of in-person lecture are...
More Info