Story
Ms. S was a direct access referral for a physical therapy assessment at United Physical Therapy. She was initially assessed on April 9, 2016.
Ms. S is a 60-year-old hand physical therapist who presents with complaints of chronic neck and upper back pain predominately on the right side. Her orthopedic history is a progression of events beginning in her early 20’s. She developed left knee pain, which she attributes to excessive running. She was diagnosed with a meniscus tear. At the age of 20, she underwent an arthroscopy for meniscal debridement and resumed her running program. Approximately 6 months later she began to develop right lumbosacral pain, which was intermittent in nature. These symptoms were complicated by an injury 2 years later related to lifting a motorcycle in which she sustained a compression fracture of the tenth thoracic vertebrae. As a result, she started to experience intermittent thoracic pain. Right lumbosacral and thoracic pain became very limiting and more constant after the delivery of her second child when she was 37. It was at this point that she developed incontinence related to running which her OBGyn told her was possibly a nerve injury. For the last ten years she has episodes of various pain patterns involving the right sacroiliac joint, neck and back provoked by load or activity. She manages all these complaints with frequent massages and limiting her activity. Her current complaint of right cervical and thoracic pain has become more constant and she has difficulty finding a comfortable position to read more than thirty minutes.
Meaningful Complaint
At the initial assessment, Ms. S’s primary complaint was right cervical and thoracic pain, which is provoked with sitting and reading. Her other symptoms of pelvic and low back pain are not currently an issue for her.
Diane’s question
Given the length of time Mrs. S has been experiencing pain, do you suspect any of her cervical or thoracic pain to be centrally mediated? What features from her story guide this clinical reasoning process?
Luci’s response
Pain is an unpleasant sensory and emotional experience that is associated with actual or potential tissue damage. Peripheral nociceptive receptors fire in response to chemical, thermal, or mechanical stimuli such as with tissue injury and inflammation, which informs the CNS via sensory pathways that leads to the conscious awareness of pain. The CNS assessment of stimuli is integrated with experiences and beliefs and a response is generated. These responses potentially include altered motor control and autonomic responses. When peripherally mediated input occurs over a significant length of time, a shift in in the threshold stimulus can occur in the CNS resulting in a sensitization in which pain is perceived without a peripheral driver.
Many sufferers of chronic pain can present with a combination of both peripheral and central mechanisms. Ms. S history consists of coping with pain for more than half her life; however, her presentation seems consistent with pain patterns that are peripherally mediated and mechanically based. During the initial interview and throughout the evaluation process, she verbalized concern and fear that the treatment might cause her chronic complaints of back pain to flare nevertheless her tolerance for assessment and treatment activities was appropriate and consistent.
Cognitive Belief
Ms. S has been a practicing physical therapist for 35 years specializing in hand therapy. She believes that her neck pain is related to a compressed cervical facet joint that is referring pain to the thoracic area. She also believes that her pelvic pain is a separate issue.
Diane’s question
How do these two beliefs relate? How does being a hand therapist relate to a compressed cervical facet joint in her mind?
Luci’s response
Ms. S has experience and knowledge assessing and treating the cervical and thoracic spine. Because of this background, her belief that her symptoms were cervical in origin were more difficult to overcome (she was ultimately determined to be a hip driver) as well as convincing her that changing alignment and biomechanics of more distal regions (hip and pelvis) would impact her neck pain and function.
Meaningful Tasks
Based on Ms. S’s story and her performance goal identified in the initial assessment, the meaningful task is to sit and read pain free for unlimited duration. The screening tasks chosen were based on the physical requirements to transition into sitting as well as sitting posture itself.
Diane’s comment on screening tasks chosen
I would suggest that low arm elevation would also be a key screening task since she has to hold a book and holding the arms up will load the neck and upper thorax, the area of her meaningful complaint.
Luci’s response
When asked to demonstrate how she sat and read at home, she assumed a sitting position with correct spinal alignment and described an extensive pillow system that supported the spine as well as her arms. As a hand therapist, Ms. S. does a lot of ergonomic assessments and I was convinced that she was unloading her arms effectively with this task. I became less interested in her arm position and loading and focused on other findings. I can see in retrospect, I should have included holding a book nevertheless.
Diane’s comment on Luci’s response
Unless her goal is to always use this ‘extensive pillow system’ when she reads, I think holding a book is very important for this case.
Luci’s response
When I reflect on my assessment choices, I recognize more than ever the tremendous amount of information that is attained and processed within a time limitation. These include all elements of the patient’s history and story, what my hands are telling me with each task, the patient’s response to each task and instruction as well as their capacity for receiving information. It is hard to pin down all of the details that guided my clinical reasoning to limiting the task progression to just sitting. I had developed my hypothesis around her hip and I wanted to see what would happen after we worked with it. I have to believe that I would have put that book in her hands for assessment if she continued to report pain with reading task in subsequent visits.
Screening Tasks
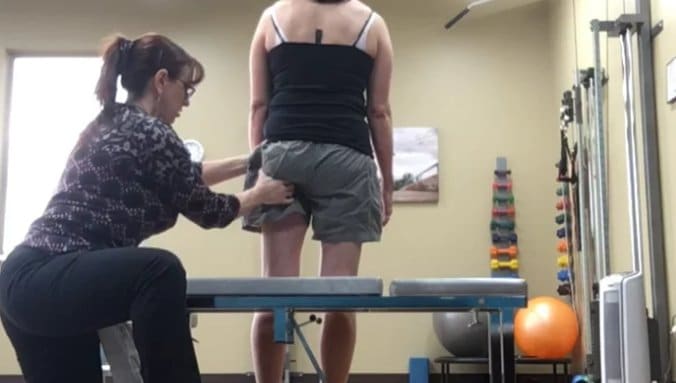
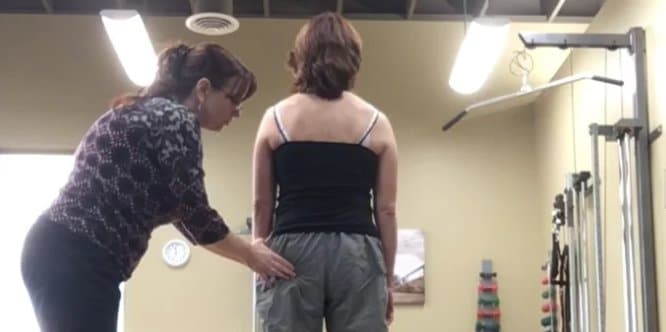
Standing Postural Screen
Even though Ms. S’s meaningful task is sitting, it is essential to assess her standing posture to determine existing postural control and alignment within and between regions as well as what strategies occur during task transitions. A painful impairment often impacts the alignment and loading tolerance of multiple regions. Optimal standing postural alignment includes a neutral pelvic girdle with no intrapelvic torsion, both femoral heads centered in the acetabulum, a smooth lumbosacral curve into a neutral thorax with symmetrical, slightly elevated, clavicles and scapulae approximated to the chest wall in slight upward rotation, and topped with a neutral head and neck.
Failed load transfer is defined as the loss of mobility, control or suboptimal alignment of a joint system within the kinetic chain and is task specific. Ms. S presented with multiple sites of failed load transfer in her standing posture. Her pelvis was rotated in the transverse plane to the right and this was associated with an intrapelvic torsion to the right and an anteriorly shifted left hip, which is congruent with this direction of pelvic torsion and rotation. Her thorax exhibited multiple ring shifts including the third and sixth ring, which were right translated, left rotated and fifth ring left translated and right rotated. Her shoulder girdle was torsioned to the right. C7 was left shifted right rotated and C2 was right shifted left rotated with her head in an intracranial torsion to the right.
Diane
Terminology question pertaining to congruence and incongruence: Given your findings above, you note that her left hip is congruent with the direction of both rotation (TPR) and torsion (IPT) of her pelvis. Can you define what congruence with respect to the TPR/IPT means independent of what congruence of the hip to the pelvis means? Give an example of an intrapelvic incongruence in your answer as well as an incongruence between the hip and pelvis.
Response
When the pelvis rotates as a unit to the left or right, it is described as a transverse plane rotation and should produce an associated intrapelvic torsion. The congruent osteokinematics of pelvic rotation in a transverse plane left and an IPT left include an anterior rotation of the right innominate relative to the left innominate as well as nutation of both sides of the sacrum relative to their respective innominate with the right side of the sacrum nutating further than the left. An incongruence of intrapelvic torsion might consist of a TPR left and an IPT right in which the right innominate anteriorly rotates relative to the left innominate but the right side of the sacrum counternutates or unlocks relative to the right innominate. In the standing screen, checking the nutation of the sacrum relative to its innominate is important to distinguish if the patient is in an intrapelvic torsion or if the pelvis is already unlocked.
Diane’s response to this response
Whenever the sacrum counternutates relative to the innominate – you no longer have an intrapelvic torsion. An IPT requires that BOTH sides of the sacrum remain nutated relative to the innominates. An incongruent TPR and IPT of the pelvis would be a left TPR and a right IPT and NO unlocking of either SIJ. This is not quite what you have described above. Let me know if these biomechanics are still unclear for you and we can take this further.
Luci’s response to the corrected congruence/incongruence terminology
Your response prompted me to review my class notes/ slides from week one:
“In a left IPT, the right innominate anteriorly rotates and the left innominate posteriorly rotates while the sacrum rotates left and nutates relative to both innominates. A right unlocking SIJ is when the right innominate anteriorly rotates and the left innominate posteriorly rotates while the sacrum rotates left and counternutates on the right and nutates on the left.”Luci’s response continued
Considering the orientation of each region and understanding the biomechanics of how each region functions together is a part of the assessment for optimal function. Body regions that are rotating opposite of each other can result in altered loading patterns that may result in developing pain and inflammation over time. A TPR IPT left of the pelvis with an anterior right hip describes the positional findings of body regions that are in congruence with each other. An example of incongruence between pelvis and hip are a TPR left with an anteriorly shifted left hip.
Diane’s response to this response
Perfectly described! And an incongruent pelvis is one that is rotated to the left in the transverse plane but associated with a right IPT.
Diane’s question
Do you think her shoulder girdle torsion (right) is congruent or incongruent to her low neck/upper thorax and why?
Luci’s response continued
The shoulder girdle and its positional relationship to the cervical and thoracic rings are another important region to assess for congruence or lack thereof. MS. S presents with shoulder girdle torsion to the right as well as a left shifted right rotated C7, which would be considered congruent with one another.
Squat
Squatting is an opportunity to assess the strategy of how load is transferred from standing to sitting. Optimal strategy for squatting includes a neutral pelvis that moves as a unit and anteriorly rotates over both hips that remain centrally seated in the acetabulum. The cervical, thoracic and lumbar postural curves are maintained with a neutral head and shoulder girdle.
Ms. S did not experience any pain during the squatting task that might influence her strategy of movement. Her pelvis started and remained in a transverse plane rotation and intrapelvic torsion to the right. The left hip started anteriorly shifted and increased anterior translation early in the task.
Diane’s question
Was there intra-pelvic control during this task? If the left hip anteriorly shifted more, would you have expected the pelvis to rotate more in the transverse plane. Any idea why it didn’t?
Luci’s response
I would expect the pelvis to rotate more. I did not process this discrepancy at the time nor during my write up. I believe that my attention was too focused on the hip.
Diane’s comment on Luci’s response
Did both SIJs remain controlled as she went through the squat? This is important to note as it will tell you if she was sitting in an IPT or an unlocked SIJ. Later you note that her right SIJ unlocked later in the squat task and her pelvic rotation reversed direction. I think it is important to include this information here.
Luci’s response
Ms. S’s pelvis remained in a TPR IPT right during the squat task within the range of squat that she performed. It was the final degrees of transition to sitting that the pelvis reversed to a left TPR and her left SIJ unlocked.
The third ring shift right and the fifth ring shift left increased late in the task while the sixth ring shift right remained the same throughout the task.
Diane’s question
Did the left hip therefore anteriorly translate before the 3rd and 5th thoracic rings translated further from their starting position?
Luci’s response
Yes
The remaining findings including the shoulder girdle torsion to the right, C7 shifted left, C2 shifted right, and an intracranial torsion to the right remained the same throughout the task.
Once all the sites of failed load transfer of a task have been identified, then further analysis must determine which site in the kinetic chain is the driver. The timing of the failed load transfer as well as the improvement in pain or perceived effort to perform the task during correction and optimization of the biomechanics are considered in this analysis.
Correction of the thoracic rings and pelvis did not improve the strategy for load transfer through the hip. Manual correction and verbal cues to obtain and maintain a centered left hip restored control of the pelvis and rings 3, 5, and 6. Therefore, the left hip is considered the driver for this task based on the timing of loss of biomechanics relative to other areas as well as the response of the other body regions to its correction.
Diane’s question
Did you get a 100% correction of all those rings, neck, cranium with just the left hip correction or did some sites remain incompletely corrected. I highly suspect that your best correction was the hip but it is likely that some upper cervical/cranial things didn’t fully correct – do you know?
Luci’s response
I didn’t comment on the cervical and cranium corrections because I did not think I could maintain a correction of the hip and reach high enough to accurately assess the cervical/cranium. I also made an assumption that if the neck and cranium improved with hip correction in sitting then it would either not change nor get worse with squatting. But that is an assumption and getting a head of myself.
Diane’s comment to this response
Neck drivers are very common for hip alignment so figuring out how you can monitor the neck and correct the hip or correct the neck and monitor the hip is extremely useful in an ISM assessment. My suggestion here would be to correct the cranium and assess what happened to C2 and C7 – what is the relationship between the cranium, C2 and C7. Once this is determined (who is the driver) assess the response of correcting this driver (or co-driver) on the TPR IPT of the pelvis. You already know that the pelvis corrects when the hip corrects so if you correct the head/neck and use your eyes to watch what happens to the pelvis you have your answer (no guessing) to what that left hip is doing. If the pelvis derotates, then the left hip is centering. Then, correct the hip with manual and verbal cues and have Mrs. S squat. Have her hold the correction and position that best allows the hip to remain centered and go palpate the cranium, C2 and C7. Ask her to stand up slowly and feel for any change in alignment of the head and neck. That will confirm whether or not the hip is reacting to the head and neck or visa versa.
Sitting
Sitting is a task of endurance. Her symptoms are produced after 20-30 minutes. Uneven load sharing contributes to excessive stress on joint and soft tissue that can result in chronic inflammation and tissue changes. The postural equilibrium must be maintained with appropriate levels of recruitment. Excessive muscle bracing or over activation can impact work efficiency and muscle metabolism leading to early fatigue. Sitting requires sufficient range of motion of hip flexion to allow the pelvis to maintain neutral alignment and equilibrium over the ischial tuberosities. The cervical, thoracic and lumbar spine must be neutrally stacked with smooth curves over pelvis without excessive muscle activation or kinks and hinging.
Ms. S presented with a transverse plane rotation and intrapelvic torsion to the right in both standing and squatting. As she assumed a sitting posture, her pelvis reversed direction into a left transverse plane rotation and the left SI unlocked.
Diane’s question
In the squatting task above you noted that her pelvis remained in the right TPR/IPT so when in the sitting task/squat did this reversal and unlocking occur?
Luci’s response
The final degrees of squatting as she sat.
Diane’s comment on Luci’s response
This finding is inconsistent with your statement above when I asked you about arm elevation as a screening task. Above, you note that “When asked to demonstrate how she sat and read at home, she assumed a sitting position with correct spinal alignment and described an extensive pillow system that supported the spine as well as her arms.” I would suggest that sitting with an unlocked SIJ with the pelvis rotated is not ‘correct alignment’?
Luci’s response
My use of the term alignment was inappropriate in this description of her support system. I would like to reword with a statement change: She positioned herself and described an arrangement of pillows that supported her trunk and arms in a manner that appeared was ergonomically supportive.
Diane’s response continued
To clarify the terminology then…. In her sitting posture her pelvis was in a right TPR and the left SIJ was unlocked (no IPT can be present because you can’t have both an IPT and an unlocked SIJ – in the first situation the sacrum is nutated relative to the innominate and in the latter it is counternutated).
Luci’s response
Ms. S presented with a right TPR IPT in both standing and squatting. In the final degrees of squat to full sitting, her pelvis reversed from a right TPR IPT into a left TPR with the left SIJ unlocking.
Her left hip started anteriorly shifted and translated further anterior as she squat and then sat.
The third thoracic ring started translated right and further translated right during the task. The fifth ring started translated left and further translated left during the task. The sixth ring started and remained right translated. Her shoulder girdle torsion and intracranial torsion started and remained right as well as the left shifted C7 and right shifted C2.
Diane’s comment
So it appears that the neck and shoulder girdles are not changing in this task – all the more reason to involve arm elevation to simulate book holding.
A transverse plane rotation of the pelvis to the left is incongruent with a left anteriorly translated hip, which was an unexpected finding so this was the first correction assessed. Manual and verbal cues to assist in centering the left hip while squatting to sit resulted in both a resolution of the left transverse plane pelvic rotation and restored control of the left SI. All of the thoracic rings shifts resolved with this hip correction allowing for neutral stacking of the spine over the pelvis, which also included the neck. C7 and C2 were restored to good alignment and control as well as the shoulder girdle and head.
Diane’s response
Wow that’s amazing that a primary driver of the hip could do all this in such a long standing patient. Not doubting you – just amazing. And in this task you were able to figure out how to correct the hip and monitor the response of the neck and head – how did you do that given your previous comments?
Luci’s response
I manually corrected the hip as she assumed the sitting position. Once she was seated, I assessed her head and neck. However, I did not ask her to resume standing which would have given me more information.
Diane’s response
Great way to do it!
Screening Task Summary
Choosing screening tasks related to the meaningful task directs the assessment to remain focused on the primary complaint and avoids distraction of unrelated findings. The goal of identifying the driver is to identify the best place to intervene in the body that is related to the patient’s goals and meaningful task.
Quick summary of Ms.S’s findings:
- Squat: primary driver- left hip
- Sitting: primary driver –left hip
Diane’s comment
But she is still armless for reading and given that this is a neck/upper thorax story with static holding of the arms as a critical part of the task I think it would have been essential to examine actually holding a book in addition to what you did above.
Vector Analysis
Once the primary driver has been identified, then more information about the underlying system impairment of the driver is required. There maybe multiple impairments involved which include articular, neural, visceral, or myofascial, all of which require very different interventions. Analysis will help us understand how to best remove the underlying system impairments that are creating non-optimal strategies so we can restore the optimal alignment, biomechanics and control for the desired goal or task.
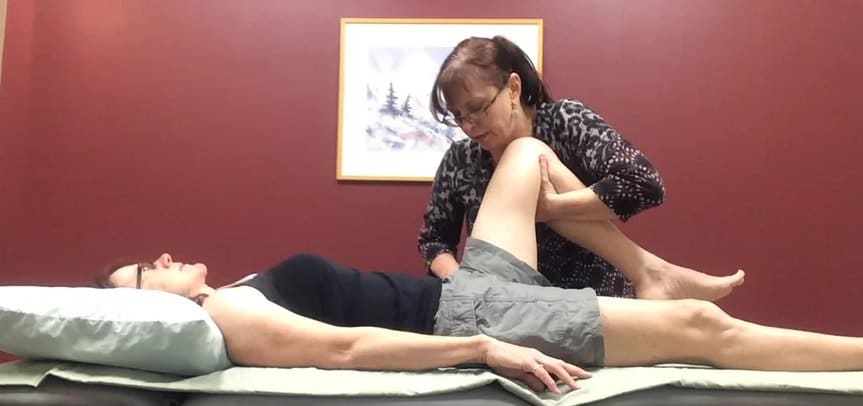
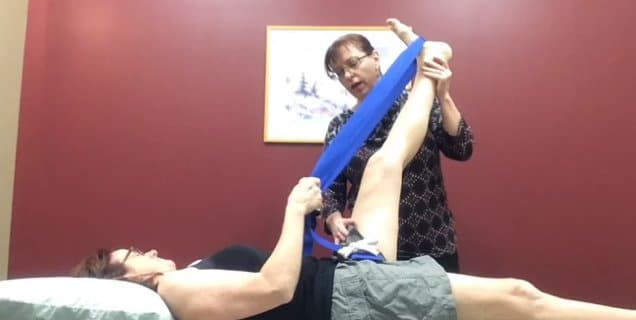
Vector analysis of the left hip was carried out in a crook lying position. The femoral head position was monitored as passive flexion was performed revealing a limitation in available ROM of less than 90 degrees.
Diane’s question
What did you perceive happen to the femoral head at the limit of the hip range? Why didn’t you examine hip rotation or abduction or extension?
Luci’s response
The femoral head and its relation to the acetabulum as well as the innominate were monitored as the hip was passively flexed. At approximately 70- 80 degrees, the femoral head lost its center and began to shift anteriorly after which point the innominate began to rotate posteriorly.
The functional hip range of motion required to sit with a neutral pelvis is primarily flexion as well as some contributions from abduction and external rotation. My focus of assessment was flexion because that is what this task required. These other planes of motion were never formally measured however in the process of release and self release, the required ROM from these other planes were addressed as well as what is important for a healthy joint system.
Diane’s response to Luci’s response
As Luci mentions, the meaningful task is sitting so unless her sitting position required abduction there was no need to examine this range of hip motion for this task and one certainly didn’t need to examine extension!
At the end range of hip flexion, a pulling restriction was identified posteriorly which was palpated to be the piriformis muscle. Upon its release, the tensor fascia lata and then the adductor were identified contributors to restriction of hip flexion.
The hip capsule and articular system were ruled out with the scour test and gliding the joint, which did not present as the limiting factor of range of motion. Vector analysis revealed loss of alignment and biomechanics to be the result of tonically over active muscles, which were neural in origin.
Diane’s question
When there are overactive muscles surrounding a joint, passive mobility tests can be misinterpreted incriminating the joint as being the cause of the restriction. How does the ‘scour test and gliding the joint’ rule out an articular system impairment? Joint gliding can be limited by all kinds of vectors so I’m unsure how this test incriminates the articular system?
Luci’s response
The assessment of the articular system is only accurate after all of the overactive muscles have been released. Once this was accomplished, glides of the different aspects of the joint capsule are performed looking for a stiff hard end feel that might be indicative of fibrosis. Winding the joint up in flexion with rotation and then compression may reproduce symptoms associated with a cartilage defect.
Hypothesis
Ms. S’s primary complaint is chronic neck and upper back pain related to sitting and reading more than 20-30 minutes. She presents with a significant limitation in available hip range of motion that does not meet the requirements necessary for sitting which results in shifting loads throughout the pelvis and spine to make the range required available. Suboptimal alignment of a static posture can potentially result in compensation and altered muscle recruitment throughout the entire spine. This hypothesis is supported by her history of injury in the left knee, which potentially contributes to origin of hip stiffness as well as the progression of chronic pain originating in the lumbosacral spine. The analysis of this history with assessment findings supports the hip as the primary driver.
Diane’s question
Ms. S also lost control of her left SIJ such that she sat with an unlocked pelvis. You didn’t perform an evaluation of her abdominal wall, pelvic floor or deep back extensors to determine if there was any dysynergies related to the primary driver i.e. the left hip. Why? Would this information have given you more guidance for your treatment plan?
Luci's response
My priority early in my treatment plan was focused on release and alignment of hip and then thoracic rings. I was interested in her TA and pelvic floor function because of her history of incontinence with running. I thought that would be considered a different task and didn’t want to change mid plan plus she was responding well with resolution of symptoms with sitting. Later I examined her muscle function with US imaging and discovered she had poor recruitment of the left side of her pelvic floor as well as a delay of left TA recruitment compared to the right. As she addressed and resolved these deficits, she did not convey that her sitting tolerance was impacted however I never specifically asked her.
Diane’s comments to Luci’s response
I agree that our initial focus in treatment should be to release and align the skeleton; however, if our treatment is to be maintained we need to know if the malalignment has been impacting the recruitment strategies particularly when there is loss of control of the SIJ. The fact that control of the left SIJ was restored when you corrected the left hip makes assessing the lumbopelvic ‘core’ muscles less necessary. IF loss of control had persisted with the left hip correction, then a full evaluation of the ‘core’ muscles would have been necessary.
Treatment Plan
The ISM treatment plan is based on releasing sub optimal strategies to restore alignment progressing towards regaining lost connections for recovery of functional movement. Identification of sub optimal strategies is based on the meaningful complaint and task defined by the patient. Ms. S’s initial treatment plan is as follows:
R: Primary driver-Left hip: piriformis, tensor fascia lata, adductors
A: Align and center femoral head- best cue was to “create space in the groin and let the sitz bones go wide”
C: Restoring femoral mobility resulted in restored control of pelvis and spine therefore additional connect cue was not indicated
M: Alignment cues were incorporated into stand to sit movement pattern
Ms. S. initially responded very well to self mobilization and release cues for her left hip; however, as her hip mobility improved, she began to experience a reoccurrence of her right sided neck and upper back pain associated with complaints of constant right SIJ pain which feels fragile and more painful as she bends forward.
Diane’s comment to this treatment response
This treatment outcome suggests that there were some things in the upper thorax and neck that didn’t correct totally with the left hip correction. I’m not suggesting that we can get it right every time! The patient’s followup story helps train our hands and eyes to know what we missed.
Luci's response
I agree with this. It was unexpected that her left hip would possibly be the driver for her neck and upper back pain. My documentation has been the observation of the most obvious findings and I am sure that I have missed more subtle findings. In fact when I reviewed the videos, I heard myself say that the thoracic rings 5 and 6 were better but not complete in their correction.
I do believe establishing the driver as the best way of where to begin is exemplified in this patient. She has received a lot of treatment over the years from many different therapists, myself included. Mobilization and release of her neck and upper back would frequently flare her right SI pain and never fully restore function. Resolving her left hip stiffness allowed us to address the thorax productively.
Diane’s response to Luci
Listening and learning from the patient’s response to what we choose to do is the fastest way to expedite expertise. Well done Luci!
Reassessment
Reassessment of Ms. S’s screening tasks revealed a new driver for her pain experience. Results are summarized as follows:
Standing posture
- Cranium: ICT right
- Thorax: Rings 6 right translated left rotated. Ring 5 left translated right rotated.
- Pelvis: TPR left Right SIJ unlocked
Diane’s question
So now instead of standing in a right IPT her right SIJ is unlocked?
Luci's response
Her TPR changed from right to left with unlocked right SIJ
Diane’s response
This post-treatment (releasing the left hip) response suggests that her motor control was tenuous and that her strategy for stabilizing her pelvis did not return to ‘optimal’ merely by releasing her hip. A few more repetitions of the squat task after releasing her left hip at the end of session one may have revealed the unlocking right SIJ. Then if time had run out, the pelvis could have been taped for support until training could begin at next session. This may have prevented the recurrence of both the neck and pelvic pain.
Squat
- Thorax: Ring 5 starts and stays left translated. Ring 6 starts and stays right translated.
- Cranium: Starts and stays in an ICT right
- Pelvis: TPR start and remain left with unlocked right SI
- DRIVER: Correction of thoracic rings 5 and 6 results in control of TPR and alignment of right SIJ
Diane’s question
what happened to the ICT, C2 and C7 – she has neck pain – don’t forget to go to the top – I think below you mention that C2 and C7 corrected – bring the information up here as well for consistency
Luci's response
Her TPR changed from right to left with unlocked right SIJ
- Thorax: Ring 5 starts and increases in left translation. Ring 6 starts and increases in right translation
- Cranium: Starts and stays in a ICT right
- Pelvis: TPR left with unlocking of right SIJ
- DRIVER: Correction of thoracic rings 5 and 6 results in alignment and control of TPR and alignment of SIJ as well as resolving ICT right to neutral
Diane’s question not addressed from last submission
did this happen in the squat as well then?
Luci's response
Yes
Initial treatment restored the left hip alignment and ROM such that Ms. S could sit with better cervical alignment however she presented with an intracranial torsion right, translation of rings 5 & 6 as well as a left transverse plane pelvic rotation and an unlocked right sacro iliac joint in all three tasks – standing, squat and sitting. Correction of thoracic rings 5 and 6 resulted in recovery of control and alignment of the cranium and pelvis.
Vector analysis of thoracic rings 5 and 6 (the current driver) reveal increased tone and overactivation of right iliocostalis fascicles to the fifth ring. The iliocostalis originates at the angle of the rib and inserts along the posterior medial iliac crest. Over activation of this muscle can result in a right rotation of the fifth ring as well as a left transverse plane rotation of the pelvis and potentially impact control of the right SIJ. Correction of thoracic rings 5 & 6 resulted in control of the right SIJ during squatting and sitting tasks as well as resolving intracranial torsion
Diane’s question
Over-activation of the right iliocostalis fascicle to the right 5th rib will cause the rib to posteriorly rotate. Can you please describe the resultant osteokinematics of the 5th thoracic ring secondary to this posterior rotation force. Include the change in position of the relevant two thoracic vertebrae, left and right ribs.
Luci's response
A posteriorly rotated right fifth rib would result in a right rotation, left translation of the fifth ring. The right fifth rib is posteriorly rotated with a translation anteromedially relative to its transverse process of the fifth thoracic vertebra while the left fifth rib is anteriorly rotated and translated posteolaterally relative to its ipsilateral transverse process. The fourth thoracic vertebrae rotates right with a left translation relative to the fifth thoracic vertebrae. At the limit of horizontal translation, the fourth thoracic vertebrae glides superiorly of its left superior costovertebral joint and inferiorly on the right costovertebral joint in an ipsilateral sideflexion. The fourth thoracic vertebrae’s inferior articular process glides inferomedially and the left inferior articular process glides superolaterally.
Diane’s comments
Luci you have, in part, described the arthrokinematics not the osteokinematics! The answer is simpler than this. The right iliocostalis attaching to the right 5th rib causes it to posterior rotate when over-active. This induces an entire ring response such that the 5th thoracic ring translates to the left, the right rib posteriorly rotates, the left rib anteriorly rotates and the T4-5 sideflexes and rotates to the right.
Diane’s question
When you corrected the 5th thoracic ring, you note that the right SIJ became controlled I’m assuming in the squat task (task wasn’t mentioned). If the activation of the right iliocostalis reduced, I can see how this could occur. How can you explain the change in the right ICT with a left 5th thoracic ring correction?
Luci's response
The dura mater is a fibrous sheath that encases and protects the spinal cord. Inferiorly, it has attachments at the sacrum and the coccyx and then superiorly at the foramen magnum and axis. The spinal dura mater is continuous with the cranial dura. The tentorium cerebelli of the cranial dura attaches along the upper edge of the petrous bone to anterior and posterior clinoid processes. The tentorium cerebelli suspends the spinal cord and dampens tensions generated from the spinal cord with the additional support from the falx cerebri. Sidebending of the cord creates tension and can induce a sidebending or lowering of the tentorium contralaterally. These tensions can influence cranial alignment resulting in torsions pulling the temporal bone medially and compress the sphenoid and the occiput into the temporal bone. Thoracic ring shifts can induce dural tension impacting cranial alignment, which are then relieved once the ring is optimally aligned.
Diane’s response
A very biological plausible response!
A new treatment plan was established to release the long vectors of the right iliocostalis and restore alignment of thorax with cues to create space between ribs and thoracic vertebrae progressing to incorporating cues with stand to sit movement.
Ms’ S was a highly motivated and extremely compliant patient whose educational background as a therapist enabled her to make rapid gains toward recovery of function within fewer visits. She was seen for a total of six visits and achieved resolution of her symptoms as they related to this task of sitting.
Diane
Great report – well done Luci!
Skills Demonstration
Case Study Author
Clinical Mentorship in the Integrated Systems Model
Join Diane, and her team of highly skilled assistants, on this mentorship journey and immerse yourself in a series of education opportunities that will improve your clinical efficacy for treating the whole person using the updated Integrated Systems Model.
We will come together for 3 sessions of 4 (4.5) days over a period of 6-8 months with lots of practical/clinical time to focus on acquiring the skills and clinical reasoning to put the ISM model into practice. Hours of online lecture and reading material and 12 hours of in-person lecture are...
More Info