Note to the reader from Diane: Courtney is trained in vestibular therapy and I am not. You will note that some of my questions are for clarity around the topic of vestibular therapy so I can better understand the outcomes/measures used in vestibular therapy to note a deficiency in performance and how improvement is measured.
Story
Mrs. B, a 56-year-old yoga therapist, attended her initial consultation on May 29th, 2020, referred by a colleague. She reported that in January she began feeling hot and unwell while travelling aboard an airplane. She walked to the end of the aircraft in hopes that the washroom would be cooler. She fainted and her left orbit struck the flight attendant’s cart. She suffered a concussion and a large contusion to the left side of her face.
Her persistent symptoms included a constant headache in the frontal region, pressure behind her left eye and left temple. She also reported a “yucky” feeling with reading, screens and scanning the environment. Mrs. B was continuing to work as a yoga therapist. She felt like her balance was very affected which made her job challenging. She noticed that when she was instructing, she would often choose the wrong word or struggle to find the correct word she wanted to express.
She was unable to seek immediate treatment due to the COVID-19 pandemic. In the past, she sought care from a chiropractor for traction after her first concussion in 2013. This concussion was due to her foothold slipping and falling, rather than fainting. Her symptoms had resolved prior to her second concussion.
Mrs. B‘s medical history was fairly unremarkable. She had asthma triggered by allergens. Notably, she had no history of neurological disorders, vestibular disorders or cardiac conditions. She had a cervical rib on her left side.
Meaningful Complaint
- Central frontal bone region headache, Left sided temple pressure and Left ear pressure
- “Yucky”/dizzy feeling with reading, screens, and scanning the environment
- Trouble finding the correct word
No pain or paresthesia were reported.
Cognitive and Emotional Beliefs
Mrs. B reported that she felt like all her symptoms were “in my head”. She often mentioned she felt “off” and she didn’t feel “normal”. She found it odd that her concussion symptoms still persisted since she understood the pathophysiology of a concussion and knew she was outside the typical timeframe of recovery.
Meaningful Tasks
- Scanning the environment with her eyes
- Reading
Diane’s question:
Did she note any difference in her symptoms when reading in sitting vs standing? I note below that you chose a standing screen to start; however, if her problem is scanning the environment whether sitting or standing, then a sitting screen may be more appropriate? However, if the symptoms differ when she scans in either sitting or standing then you may have two start screen positions that pertain to each screening task.
Courtney’s response:
I always do the full oculomotor screen in sitting for safety reasons. I chose standing as her start screen as there was no difference in the patient’s experience or alignment in sitting versus standing and it was easier to find the driver in standing.
Screening Tasks
A standing screen was performed for a baseline to understand Mrs. B’s natural starting position.
Her meaningful tasks were reading and scanning the environment; therefore, horizontal saccadic eye movement was chosen for her screening task as it is involved in both tasks. Horizontal saccades are a quick, simultaneous, bi-ocular movements where the eyes jump between two fixed targets.
Standing Screen
A standing screen was chosen to give us an idea of her starting position prior to layering on any tasks. This gave us an indication of whether she started with suboptimal alignment and control and whether her strategy improved with the task or continued to be suboptimal.
Diane’s question:
The current research on posture and movement suggests that alignment is irrelevant to task performance (1). In the statement above, the words ‘suboptimal alignment’ are used, which suggests you believe that optimal vs suboptimal alignment can be determined. What is your belief system around alignment (optimal vs suboptimal) and why?
Courtney’s response:
Many people have asymmetries and rotations in their body from habitual patterns they have developed over the years. These are often described as sub-optimal as they vary from the textbook definition of “posture” or “alignment”. However, having these asymmetries and rotations in different regions of the body doesn’t necessarily mean they are dysfunctional or pathological.
Diane’s comment:
And I might add it doesn’t mean they are responsible for the patient’s symptoms. This would require further testing.
Courtney’s response continued:
Suboptimal alignment becomes relevant when it limits the appropriate biomechanics and/ or impacts control during function. For example, in this case, Mrs. B’s cranium was resting in a suboptimal alignment in standing. Furthermore, when she performed her meaningful task of eye tracking, her suboptimal alignment worsened and her task suffered. If correcting cranial alignment improved her saccadic eye movement then her suboptimal alignment becomes relevant and needs to be addressed. This method of assessment and treatment of alignment is much more task and patient specific.
Diane’s response:
This is exactly right – patient specific assessments to determine if/when our findings are relevant to the clinical picture!
Findings for the Standing Screen
Functional Unit #1
Pelvis: Mrs. B’s pelvis was rotated to the left in the transverse plane with a congruent intrapelvic torsion, meaning her left innominate was posteriorly rotated, her right innominate was anteriorly rotated and her sacrum was rotated left and nutated relative to both innominates.
Diane’s question:
Well described! In ISM, we use the term congruent in two ways. What are they and which definition are you using above?
Courtney’s response:
The definition of congruence I am using above is an intraregional form of the term congruent. This refers to the osteokinematics of the pelvic bones that corresponds with a transverse plane rotation of the pelvis.
In ISM, we also describe inter-regional congruence which corresponds to appropriate alignment between two regions of the body. For example, if the pelvis is rotated to the left in the transverse plane, I would expect the right hip to sit more anterior in the acetabulum if they shared a congruent relationship.
Furthermore, the alignment of the body needs to be congruent to the task. For example, if a hockey player shoots right then the shoulder girdle should be rotated to the right to be congruent to the task during the wind up.
Diane’s comment:
The two types of congruence in ISM are:
- One body region is positioned and/or moving accordance to the requirements of the task (all three of your paragraphs above)
- Two body regions are positioned and/or moving in the same direction regardless of the task
The first sentence of the second paragraph is one type of congruence and the second sentence in the second paragraph is the second. The right hip isn’t rotated to the left in the transverse plane in this example, it is sitting more anterior in the acetabulum relative to the left hip (reader see below) – this is congruent with what would happen in a left TPR of the pelvis but the two body regions are not ‘rotating in the same direction’.
Diane’s question:
So, given that information can you give me an example of an incongruence of each type?
Courtney’s response:
An example of an incongruent relationship regardless of the task would be if the pelvis was rotated to the left in the transverse plane, as in Mrs. B’s case, but the left hip was sitting more anterior in the acetabulum relative to right hip. This suggests there is likely two drivers: one that is rotating the pelvis left and another that is translating the left head of the femur anterior in the acetabulum.
An example of a task specific incongruent relationship would be the relationship between Mrs. B’s upper thorax and the meaningful task of cervical rotation to the left. If this was her meaningful task, the orientation of her second thoracic ring, which was rotated right and translated left, was resting in a suboptimal alignment for this task. During head and neck rotation left, the second thoracic ring should rotate to the left and translate to the right. If the second thoracic ring remained rotated right and translated left, this would be suboptimal alignment and biomechanics for the task and therefore, it was an incongruent relationship to cervical rotation left.
Diane’s comment:
Well described.
Hip: Mrs. B’s right hip was translated anterior relative to the acetabulum. This was congruent to her pelvic alignment.
Thorax: Her seventh thoracic ring was translated left, rotated right. Her sixth and eighth rings were translated right, rotated left. This pattern of thoracic ring position is called a sandwich and resulted in a net left rotation of the lower thorax.
Diane’s question:
Which of these thoracic rings is/are congruent with the rotation of the pelvis and which is/are incongruent? How does determining this help in the decision process for finding drivers, or priority regions of the body for further assessment?
Courtney’s response:
Mrs. B’s 6th and 8th thoracic rings are congruent with her pelvis meaning they are rotating in the same direction as the pelvis. Her 7th ring is rotated to the right, translated left which is incongruent to the pelvis. For my assessment, I am interested in where the incongruence lies within and between regions of the body. I am looking for twists in the system where things potentially could be going wrong. Further into the assessment, I assessed the impact on alignment, biomechanics and control of other areas of the body and the task when I corrected the incongruent rotations. If these corrections improved other regions and the task they became a priority for further evaluation and treatment.
Functional Unit #2
Cervical Spine: Mrs. B’s C7 was congruent with her upper rings with a right rotation and left translation. Her C5 and C6 were rotated to the left, translated right.
Thorax (Rings 1 & 2): Her first thoracic ring was rotated right and the second thoracic ring was translated left, rotated right which resulted in a net rotation of her upper thorax to the right. (The first thoracic ring does not translate when it rotates due to the anatomy of the costovertebral joints of this ring).
Cranial region: Mrs. B’s cranium rested in an intracranial torsion right with an incongruent sphenoid rotated to the left. Her C1 was rotated to the right and C2 was rotated to the right, translated left.
Shoulder girdles: Mrs. B’s shoulder girdles were congruent with her upper rings and lower cervical spine. They were rotated to the right in the transverse plane. Her left head of humerus was slightly more anterior relative to the glenoid than her right. Her left clavicle was anteriorly rotated and the right was posteriorly rotated. Her manubrium was rotated to the right and laterally flexed right.
Diane’s question:
If we can say that all these findings for standing are ‘suboptimal’, which of those noted in this functional unit #2 are you most interested in and why?
Courtney’s response:
I am most interested in the cranial region as there was an incongruent alignment between her sphenoid and her temporal and occiput bones. All other regions were congruent with each other; therefore, a correction of her incongruence should improve the alignment of the other regions.
Diane’s comment:
Given her left orbital trauma, this is a logical and probable hypothesis.
Functional Unit #3
Knees: unremarkable
Feet: unremarkable
Diane’s question:
If the pelvis is rotated to the left and the right hip is anterior to the left as noted above, where would you expect the resting position of the left and right foot to be (i.e. one should be more pronated and the other supinated if they are able to adapt to the descending rotation force). When you say unremarkable, do you mean they are congruent with the rotation of the pelvis, or were they in neutral alignment. Which is more remarkable and why?
Courtney’s response:
Yes, the feet were congruent with rotation of the pelvis. Her right talus was resting more adducted and plantar flexed relative to the calcaneus. Her right calcaneus was laterally rotated relative to her talus which positioned her right hind foot in more pronation relative to her left hind foot.
It would be more remarkable if her feet were resting in neutral as this would be incongruent to the alignment of the pelvis.
No drivers were identified in standing as this was performed as a baseline.
Horizontal Saccades Assessment
I based the screening task on what was meaningful to the patient. For Mrs. B, her meaningful tasks were reading and scanning the environment with her eyes. Both of these tasks involved horizontal saccadic eye movements; therefore, the screening task chosen was a fixed target, horizontal saccade test. This test is common to baseline oculomotor screens. Horizontal saccade testing is an assessment of an individual’s ability to jump their gaze between two static targets. This requires adequate muscle activation of her extraocular musculature, stability muscles of the craniovertebral region and normal cranial nerve function, as well as appropriate higher order processing for memory, and predictive eye movements.
Diane’s question:
Is there a different test for smooth eye scanning as opposed to saccadic and does it matter? i.e. same processes involved in both tasks?
Courtney’s response:
Smooth pursuit involves much more higher order processing so I chose fixed saccades for that reason.
Mrs. B was able to complete 3 seconds of horizontal saccadic eye movement accurately before her eye movement became hypometric. This means her eyes were undershooting the target and needed another movement to locate the target. Not only did this test reproduce her dizzy symptoms, the change in eye function during the task coincided with the onset of her dizziness.
Diane’s question:
Was this task done in the standing position? Why would sitting require a different starting screen analysis?
Courtney’s response:
I always do oculomotor testing in sitting initially for safety. Once I know there are no red flags and it doesn’t provoke intense symptoms, I repeat the test in standing so I can assess changes in regions of the body more easily. There was no difference in the performance of the task or symptom severity between sitting and standing.
Diane’s further comment/question:
My question here is directed more to the impact of a poorly controlled SIJ on the cranium and thus this test. If Mrs. B had poor control of her pelvis, and this wasn’t considered there could be a difference in the test results that had nothing to do with her cranium but rather be influenced by changes in her pelvic floor strategies and then dural tension to the cranium.
Findings for the Horizontal Saccades Assessment
Functional Unit #1
All regions in functional unit 1 remained in status quo as the standing screen during the task
The region of best correction for the sites of impairment in functional unit 1 was the thorax. A three ring thoracic ring correction of thoracic rings 6, 7, and 8 resulted in de-rotation of the pelvis and centering of the right hip. Conversely, a correction of her pelvis or hip alignment did not change the alignment of the lower thorax. Therefore, the thorax was the region of best correction for functional unit 1.
Diane’s question:
In ISM, a driver must not only improve alignment, biomechanics and/or control of other sites of impairment, it must also improve the patient’s experience and performance of the screening task. Was Mrs. B able to complete a longer duration of horizontal saccadic eye movement accurately before the movement became hypometric when her lower thoracic rings were corrected?
Courtney’s response:
Her screening task was not reassessed at this stage as she reported that this thoracic ring correction increased the baseline of her symptoms. This finding suggests that although the thorax corrected other sites of impaired alignment, it is not the driver for her task or her meaningful complaint.
Diane’s comment:
Because her symptoms were worsened with this correction, I would suggest that, as you say, you haven’t found the driver yet! Correcting biomechanics and alignment is not enough for determining alignment and this is a key point – the patient’s experience must improve too. On to functional unit #2!
Functional unit #2
Cranial: Her intracranial torsion right increased after 3 seconds of eye tracking. C2 increased its translation left, rotation right. Her sphenoid remained rotated left.
Cervical Spine: C7 remained translated left and rotated right.
Thorax: TR1 remained rotated right and TR 2 remained translated left and rotated right.
Shoulder girdle: remained congruent to the upper thorax, rotated to the right.
Driver for functional unit: A co-correction of the sphenoid, occiput and temporal bones (cranial region) aligned both the cervical and upper thoracic spine. The shoulder girdles followed the de-rotation of the upper thorax and aligned with the cranial correction. Reassessment of the task revealed that the time to onset of symptoms with this cranial correction increased to 30 seconds, from 3 seconds. Furthermore, the patient reported feeling the performance of the task was much easier and was able to move her eyes faster between targets.
Diane’s question:
You note that she was able to move her eyes ‘faster’; however in the screening task you emphasize target accuracy and length of time. Was she able to maintain accurate tracking faster and for longer? Are they a different measure and imply different mechanisms?
Courtney’s response:
Her being able to move her eyes “faster” was a subjective finding as I did not have a way of quantifying the speed. Due to my position when doing a cranial correction, I relied heavily on the patient’s subjective response to the correction as the symptoms correlated to the onset of hypometric saccades. In future case studies, I would include infrared technology for objective data on eye tracking.
Functional unit #3
All regions of functional unit 3 remained in status quo during the task.
It should be noted that a full oculomotor screen, cranial nerve assessment and cerebellar examination were performed and revealed nothing remarkable other than the hypometric saccades. She also had negative vertebrobasilar artery insufficiency test.
Summary of Screening Task – Horizontal Saccadic Eye Movement:
The cranial correction in functional unit 2 corrected the lower thorax, which corrected all other areas of impairment in functional unit 1, and all regions of functional unit 3. The patient experienced ease of eye movements and a significant reduction in her dizzy symptoms. As these symptoms previously correlated with the onset of her hypometric saccades, an assumption was made that if her experience was changed, her performance during the eye tracking task would also be improved.
Diane’s comment:
ISM tries to eliminate assumptions and test hypotheses. If I understand what you have written correctly, her performance of the task improved and she noted less effort to perform the requested screening task, no assumptions here!
Further Analysis of the Drivers: Cranial region – sphenoid, occiput, temporal bones
Active Mobility (tested during head and neck rotation): Mrs. B had reduced rotation of the head and neck to the left. Her right temporal bone did not anteriorly rotate when turning her head to the left. Normal biomechanics of the cranium when turning the head to the left is that the left temporal bone posteriorly rotates and the right temporal bone anteriorly rotates.
Diane’s question:
- What should the occiput do osteokinematically and what should happen arthrokinematically at each occipitoatlantal joint (i.e. note the appropriate glides) in left head and neck rotation?
- If the head is neutral in the transverse plane (not sideflexed or rotated as a ‘ring’ or unit’ in space AND the temporal bones and occiput are in a right ICT and C2-3 is translated left/rotated right, where is the atlas in relationship to the occiput. Where is the atlas in relationship to C2 (just osteokinematically, not arthro at this point!)
Courtney’s response:
Each occipitoatlantal joint is comprised of a superior-medial oriented concave articular surface on the atlas and a respective inferior-lateral oriented convex condyle of the occiput. The joint surfaces also diverge posteriorly, or converge anteriorly.
-
- a.) Osteokinematically: the occiput should have a contralateral lateral flexion (right) coupled with left rotation when the head and neck rotates left.
b.) Arthrokinematically, during head and neck rotation left, the left occipital condyle travels posteriorly relative to the superior articular facet of the atlas. Simultaneously, the right occipital condyle glides anteriorly relative to the superior articular surface of atlas.
- a.) Osteokinematically: the occiput should have a contralateral lateral flexion (right) coupled with left rotation when the head and neck rotates left.
- I would expect the atlas to be translated right, rotated left to unwind the rotation between the occiput and C2-3.
-
Diane:
Agreed except it doesn’t translate at all, why?
Courtney:
The transverse ligament attaches the atlas to the dens of the axis and will tension during rotation of the axis. It will not allow translation of the atlas unless there is loss of structural integrity to the ligament. Therefore, assuming the transverse ligament is intact, if the atlas is translated osteokinematically, it is driven by the position of the axis below. It cannot arthrokinematically translate relative to the axis.
Diane’s response:
Correct. And arthrokinematically during left rotation of the atlas relative to the axis the right inferior condyle of the atlas glides anterior and inferior and the left inferior condyle of the atlas glides posterior and inferior.
Passive Mobility Testing including Analysis of Vectors: A correct, release and listen technique was used where the sphenoid was decompressed from the sphenosquamosal suture on the left and rotated in the transverse plane to neutral followed by distracting the temporal bones from the occiput at the occipitomastoid suture and de-rotating temporal bones to neutral. Upon releasing this correction, attention was paid to which bone moved first and in which direction it moved. Here, the greater wing of the left sphenoid moved first into left rotation and approximated the squamous portion of the temporal bone which compressed the sphenosquamosal suture. This first listening was strong, meaning that it was hard to decompress the sphenosquamosal suture and the left rotation began immediately and forcefully when the correction was released. The sphenoid not only rotated to the left but additionally, the left greater wing of the sphenoid pulled inwards at the end of the movement. This was likely created by an intracranial vector from the left anterior cerebellar tentorium hypothesized to be caused by congestion in the venous sinus of the left anterior cerebellar tentorium. As the two layers of the cerebellar tentorium distend, a vector of pull is created where the left anterior cerebellar tentorium attaches at the petroclinoid process of the sphenoid.
Diane’s question:
What did you feel that made you conclude the vector was inside the cranium? The temporalis muscle can also do this, so I’m curious as to how you would differentiate an over-active temporalis muscle compressing the sphenosquamosal suture from the anterior cerebellar tentorium.
Courtney’s response:
Firstly, when I decompressed the sphenosquamosal suture, the resistance was not myofascial in nature; it had a quality of hydrodynamics. When correcting Mrs. B’s sphenoid, it felt more like there was a resistance similar to the feeling of pushing water or lifting a pool cover off the surface of the water.
Diane’s comment:
Nice metaphor for what this feels like!
Courtney’s response continued:
Secondly, after correcting, releasing and listening, there was a strong pull inward at the end of listening. The pull continued along the line of the left petroclinoid ligament into the cranium. I confirmed this with a cerebral falx listening which is a Barral technique used to assess for intracranial restrictions. This resulted in a listening that pulls into the left anterior cerebellar tentorium.
We can rule out any articular restrictions of the bilateral occipitoatlantal joints and the cranial sutures as I was able to fully correct the alignment of the sphenoid, occiput and temporal bones. If there had been articular restrictions, the arthrokinematics of these joints and sutures would have been disrupted and a complete correction to neutral would not have been possible.
The second listening was less strong and started with the left temporal bone anteriorly rotating followed by the right temporal bone posteriorly rotating. The listening did not travel down into the neck. Just as above, there is a short inward drawing of the right temporal bone at the end of the movement. Again, a cerebral falx spring was used to confirm intracranial vectors and there was a hydrodynamic quality to the correction and listening.
Diane’s question:
Because you could completely correct the cranium (sphenoid, temporal bones and occiput) this finding rules out an articular system impairment. Which joints within the cranium and between the cranium and neck are ruled out as being restricted?
Courtney’s response:
We are able to rule out articular restrictions between the occipital condyles and the superior articular surfaces of the atlas at the bilateral occipitoatlantal joints. We can also eliminate articular restrictions at the sphenosquamosal and occipitomastoid sutures of the cranium.
Diane’s further comment and question:
When there is an incongruent rotation within the cranium, such as in this instance (sphenoid rotated left and ICT to the right), there are at least two vectors. One you have identified as being the left anterior cerebellar tentorium, which appears to be compressing the sphenoid into the temporal bone at the sphenosquamosal suture. What structure(s) caused the second vector/listening. These would be in relationship to the temporal bones and occiput.
Courtney’s response:
One structure that spans between both petrous portions of the temporal bones is the posterior cerebellar tentorium. This tentorium encloses both the transverse and sigmoid sinuses which, if enlarged due to venous congestion, has the potential to tension the tentorium. This is explained further in the hypothesis.
Active control test: none
Passive control test: none
Falx listening: This is an osteopathic technique to assess the tension in the intra-cranial dural membranes that can change with pressure changes in the dural venous sinuses. Mrs. B’s falx felt very full. Upon release, there was a listening into left anterior cerebellar tentorium then right posterior cerebellar tentorium.
Diane’s question:
What does a ‘very full falx’ feel like? Can you describe this for someone who has never felt this before? The superior sagittal sinus is what is full and then tenses the two layers of dura that form the cerebral falx.
Courtney’s response:
A very full falx feels hard like a coconut. It is very hard to approximate hands during the falx listening technique. There is a hydrodynamic quality to the movement, like compressing an overfilled firm water balloon.
Hypothesis
The biomechanical forces that result in a concussion cause overstretching of the axonal portion of the neural cells which results in a disruption of the neural cell membranes (2).
This microtrauma creates a series of neurochemical changes, metabolic shifts and an influx of inflammatory cells. The consequence of these mechanisms is the increase in pressure within the cranium which slows cerebral blood flow by up to 50% (2,3). These changes in physiology should resolve rapidly in the first 14 days then completely resolve in approximately 30 days (3,4). However, for a small subgroup of mild traumatic brain injuries, symptoms persist past the above time frames. Therefore, these processes alone, cannot account for the persistent symptoms.
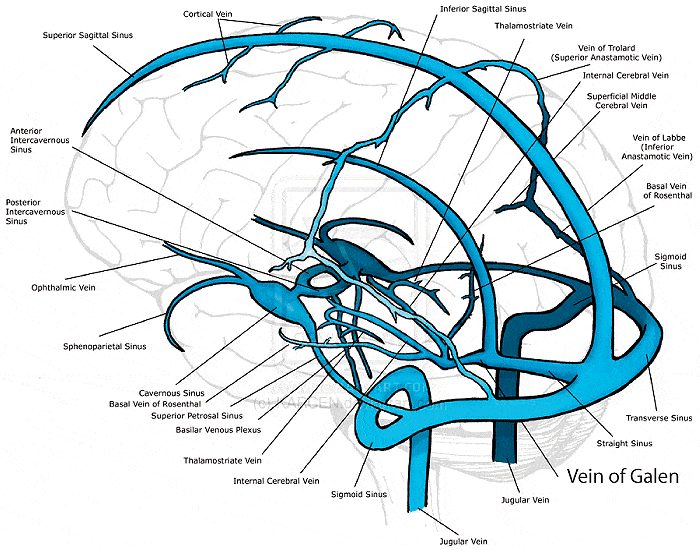
The venous drainage for the cerebrum, cerebellum and brainstem empty into dural venous sinuses via veins. The veins draining from various parts of the cerebrum drain into the superior sagittal sinus, cavernous sinus or the transverse sinus. Interestingly, these three sinuses converge into the sigmoid sinus and drain terminally into the internal jugular vein. (5)
The internal jugular vein exits the base of the skull via the jugular foramen. This foramen is located bilaterally between the occiput and temporal bones.
With an intracranial torsion to the right, the right temporal bone is posteriorly rotated and the left temporal bone is anteriorly rotated relative to the occiput. The rotation of the temporal bones changes the shape of the jugular foramen with the potential to reduce the efficiency of the venous drainage from the sinuses contained by the dural membranes.
Diane’s question:
I don’t know the answer to this question!! Is the jugular foramen reduced more by anterior or posterior rotation of the temporal bone, or equally by either?
Courtney’s response:
When looking at anatomical studies in cadavers, the jugular foramen is a triangle shaped orifice with the pars venosa located in the posterolateral portion. This pars venosa contains the internal jugular vein, three cranial nerves and the posterior meningeal artery (6). Due to this orientation, I would hypothesize that the portion of the jugular foramen most relevant to this pathology is compromised with a posterior rotation of the temporal bone. This would compress the posterolateral aspect and, therefore, impact the patency of the internal jugular vein and reduce the dural venous drainage.
Diane’s comment:
So when there is a right intracranial torsion, the posterolateral part of the right jugular foramen could potentially be compressed. I haven’t actually correlated over time the side of the posterior cerebellar congestion with the direction of an ICT – something to look into!
If drainage is slowed, there is the potential that the venous blood will pool in the sinuses as this is a valve-less system. This can create a back flow of pressure into the sinuses. This can impact the cranial nerves that control horizontal movements of the eyes (CN3, 4, 6) that traverse the cavernous sinus. Also, as this is a dural venous system, the increase in pressure has the potential to increase dural tension. Both the oculomotor and abducens nerves have intradural segments as well as interdural segments where the cranial nerves pierce the walls of the venous sinus (7,8). This increase in dural tension can tension the cranial nerves resulting in changes in motor function.
Diane’s comment:
How cool is that! I had no idea the anatomy of CN 3 & 6 being intradural. The veins of these nerves could potentially be significantly impacted if the pressure in the venous sinuses rose higher than the intra-neural venous pressure.
Along with the backflow of pressure, Mrs. B’s condition is further complicated by the incongruent sphenoid rotation from striking her orbit on the cart. This can further increase pressure in the cavernous sinus as its inferior border is the greater wing of the sphenoid. It may also increase tension of the dura of the cerebellar tentorium as it has fixed attachments to the temporal bones and the posterior and anterior petroclinoid processes of the sphenoid (9).
This incongruent sphenoid orientation and intra-cranial rotation is likely why there is a subgroup of post concussive patients that do not respond to conventional treatment.
Diane’s comment and further question:
Whenever a trauma occurs to the body a threat occurs. Our natural reaction to threat is to respond with the ‘fight or flight’ response and part of this involves the sympathetic nervous system. Think about the innervation of the venous system in the body and can you propose an alternate hypothesis that could help to explain the persistence of this condition beyond the expected recovery timeline?
Courtney’s response:
The sympathetic nervous system has the capacity to increase the contractile tone of the smooth muscle of the venous system causing vasoconstriction. This vasoconstriction could slow the drainage of the venous sinuses resulting in a backflow of pressure in the cranium. There are neuroradiological studies that demonstrate that there are cerebral blood flow changes acutely and chronically post mild traumatic brain injury (10).
The reason I did not choose this as my primary hypothesis is that I would expect the backflow of venous blood flow to be much more general and bilateral. For Mrs. B, her falx listening suggested venous pressure in the region of her left anterior and right posterior cerebellar tentorium. This diagonal pattern of tension/pressure suggests a twist in the system rather than a general back flow of pressure. Also, Mrs. B did not present with any other classic signs of paroxysmal sympathetic hyperactivity such as increased respiratory rate or heart rate, hyperthermia; however, these were not objectively measured.
Diane’s comment:
Well-reasoned.
Treatment
Mrs. B’s treatment plan followed the principles of the Integrated Systems Model where initially the driver of the task is released/aligned and then strategies are taught for a more optimal movement. The order Release, Align, Connect and Move was followed as often motor control improves once more optimal alignment and biomechanics are achieved. If the motor control strategy does not improve, then we need to specifically retrain a new strategy to maintain optimal alignment, biomechanics and control throughout a task. In ISM, treatment is initially directed to the driver, which in this case was the cranial region, namely the cranium.
Based on the hypothesis described above, we asserted that Mrs. B’s symptoms and impaired saccadic eye movements stemmed from cranial nerve dysfunction (CN3, 4 & 6) secondary to increased dural tension as a result of venous back flow caused by her intracranial torsion. Therefore, the goal of our treatment was to improve neural function by improving arterial flow, and venous drainage by releasing vectors holding the cranium and sphenoid rotated incongruently. Releasing theses vectors would improve the alignment of her cranial region which, in turn, would improve the task and the patient’s experience. These vectors were identified as intracranial, meaning they stemmed from inside the cranium. For this reason, osteopathic techniques taught by the Barral Institute and integrated with ISM were used to address the dural tension.
Release
Intracranial releases:
- Left anterior cerebellar tentorium release
- Right posterior cerebellar tentorium release
Diane’s comment and further question:
Can you describe the technique you used to release the cerebellar tentorium both at its anterior left and posterior right location, as this technique may not be familiar to all readers. Please include in your response not just ‘what you do’ but what you wait for while you are doing the release and how you know before you even test the meaningful task if it has been successful.
Courtney’s response:
Anterior cerebellar tentorium release:
I used a Barral technique taught in Part 3 of the ISM series. This technique was performed with the patient supine and the therapist working on the cranium at the head of the treatment table.
For Mrs. B, we wanted to release the left anterior cerebellar tentorium so my left hand stabilized the temporal bone and the right hand distracted the greater wing of the sphenoid. With my left hand, I stabilized the temporal bone by placing my thumb (with permission) in the external auditory meatus and wrapped the radial side of my index finger onto the mastoid process to stabilize with a pinch grip. The pads of my right index, middle and ring fingers landed on the greater wing of the sphenoid on the left side. To perform the technique, gentle pressure was applied to pull the temporal bone laterally and simultaneously distract the greater wing of the sphenoid at the sphenosquamosal suture. I fanned this distraction to find the direction of greatest restriction and then held the distraction and waited. I waited until I felt the resistance melt away and the sphenoid and temporal bones float apart. To ensure I got a good release of the anterior cerebellar tentorium, I rechecked the resistance met when trying to distract the sphenoid from the temporal bones during the correct, release and listen technique. Furthermore, reassessment of the falx listening technique revealed that there was no longer a pull into the left anterior cerebellar tentorium which affirmed that the technique had been successful.
Posterior cerebellar tentorium release:
Again, the philosophy for the technique used is from the Barral Institute and the technique was taught during Part 3 of the ISM series. The objective of this technique was to drain the cranium through the sigmoid and transverse sinus via the jugular vein at the jugular foramen.
The patient remained supine with the therapist at the head of the table. To release the right posterior cerebellar tentorium, my right hand used a V-spread technique where my right index finger rested on the mastoid process of the temporal bone and my middle finger on the occiput. The heel of my left hand was placed on the contralateral (left side) of the frontal bone. Firstly, I spread my index and middle finger to distract the temporal bone from the occiput at the occipitomastoid suture. Secondly, gentle pressure was applied with my left hand directed towards the right jugular foramen. Finally, I waited for the sensation of the temporal bone distracting laterally from the occiput on the right side. This often feels like a sensation of something “letting go”. If you have ever used a French press, it is similar to the feeling when you begin to compress the coffee. You meet a small amount of resistance from the surface tension of the liquid, then you can smoothly push the plunger down. We are much more gentle with the cranium than the French press but it feels similar. (Diane’s comment: Love this description! Yes!!)
Once I felt the temporal bone distract from the occiput, I rechecked the correct, release and listen technique. If the cranium has been drained successfully, you will noticed there is much less resistance when trying to correct and there will be no listening drawing inward upon release. I used this technique prior to rechecking the task to ensure the intracranial vectors had been eliminated. Again, reassessment of the falx listening technique was used to affirm a good release of the cerebellar tentorium had occurred.
Once the initial intracranial vectors were released, the correct, release and listen technique was reassessed. Firstly, it was noted that the sphenoid was now congruent with the temporal bones, meaning that the right temporal bone was still posteriorly rotated relative to the left and the sphenoid was rotated right in the transverse plane. This meant that the sphenoid no longer needed to be decompressed at the sphenosquamousal suture on the left. If the intracranial tension was the only thing driving the position of the cranium, I would expect the cranium to be resting in neutral. It was also noted that it was much easier to align the temporal bones. There was no hydrodynamic quality which was previously felt. Upon release of this correction, the pull was extracranial, meaning the vector causing the ICT right was felt on the outside of the cranium and it pulled into the neck. This listening had an elastic quality which is consistent with a neuromuscular vector. The pull followed the line of the right upper fibers of trapezius and semispinalis capitis.
Extracranial releases for upper trapezius and semispinalis:
The release technique used is called Release with Awareness. This technique involves shortening the overactive fascicle(s) of the target muscle to reduce muscle spindle excitability. Cues are then layered on to further reduce tone of the fascicle through the principle of descending inhibition. In this case the cue “find this spot under my thumb in your brain and try to let it melt away” was used. Mrs. B’s yoga background made her very familiar with conscious relaxation techniques and this was very effective. Finally, the muscle fascicle is taken through its full range to re-establish muscle length.
Align:
After the intracranial and extracranial releases were performed, Mrs. B’s sphenoid, temporal bones and occiput rested in neutral while laying supine. There were no vectors pulling on the cranium to cause an intracranial torsion.
When we changed Mrs. B’s position to sitting to reassess her task, her cranium drifted back into a subtle intracranial torsion right. There was no vector pulling her into this position but the weight of her head and gravity seemed to cause her to drift back into her previous habitual position.
Using the cue, “increase the space behind right ear”, Mrs. B was able to align her cranium and maintain that position in sitting.
We reassessed Mrs. B’s horizontal saccadic eye movement in sitting. Her saccadic eye movement didn’t fatigue until ~30 seconds, again this coincided with the onset of her symptoms. She reported a significant increase in ease of movement and speed between targets.
For homework, Mrs. B worked on improving her alignment by using the cue “increase the space behind right ear” and holding for 10 seconds hourly.
Because her eyes still fatigued, there was a need to implement some sensorimotor retraining. This eye movement piece was addressed in our later sessions.
Followup treatment sessions
Subjectively, Mrs. B had a very positive response to her initial treatment. She reported reduced intensity and frequency of dizziness and her “yucky” feeling. The pressure behind her left eye had resolved since her first appointment. She still suffered from frontal headaches and used incorrect words when teaching yoga. Her meaningful complaints were still triggered by eye tracking activities such as reading, using screens and scanning the environment so we continued to use horizontal saccadic eye movements for her meaningful task.
Objectively, at her second appointment, her sphenoid was resting congruent to occiput and temporal bones; meaning, rotated right in the transverse plane. She retained this congruent alignment after her treatment from her initial consult which is likely why the pressure behind her left eye had resolved. However, her temporal bones and occiput drifted back into an intracranial torsion right which likely accounted for her lingering symptoms.
During her meaningful task of horizontal saccadic eye movements, she had reduced perceived effort and symptoms during the task. Objectively, she was able to perform 30 seconds of saccades before they began to fatigue and become hypometric. This means that her gains from her initial consult were maintained to her follow up. Simultaneously, at 30 seconds her cranium began to increase the right intracranial torsion and her dizziness symptoms started to increase in intensity. The cranium was still the primary driver for her fatiguing horizontal saccades; therefore, a vector analysis of the cranial region was performed.
I repeated the correct, release and listen assessment for Mrs. B’s cranium. Her cranium felt much easier to correct this week, meaning there wasn’t as much hydrodynamic resistance as described previously. When the cranium was released, the initial listening was on the right side. The temporal bone posteriorly rotated relative to the occiput and pulled inward indicating an intracranial vector. During the falx listening assessment, similar findings were found, as the cranium didn’t feel as full or firm and the listening followed the right cerebellar tentorium.
New this week, she had an overactive right sternocleidomastoid on a second listening after releasing the intracranial vectors.
Treatment:
Again, we followed the principles of ISM treatment where we released the vectors creating a suboptimal alignment prior to progressing her movement retraining.
Release:
At this session, we released her right posterior cerebellar tentorium, with the same Barral technique described above, as that was the initial listening during the further assessment of the driver. A release with awareness was performed on her right sternocleidomastoid as this was the second listening after releasing her right cerebellar tentorium. Interestingly, the nerve supply to sternocleidomastoid and upper trapezius come from the spinal-accessory nerve which is the eleventh cranial nerve. This nerve exits the cranium at the jugular foramen, therefore it is likely that these muscles are reacting to a compressed nerve supply as the spinal-accessory nerve traverses the right jugular foramen.
Align:
After all vectors pulling her cranium into an intracranial torsion right were released, she still had a subtle ICT right when returning to the sitting position and required the same cue of “space behind right ear” to achieve optimal alignment.
Her meaningful task was reassessed with the “space behind right ear” cue and she was able to maintain optimal alignment without fatigue for 30 seconds and without any reproduction of her symptoms. She reported that it was mentally taxing as she had to really focus on the position of her cranium, otherwise she could feel symptoms returning. She found it helpful to place her fingers on her mastoid processes for tactile feedback that she was performing the task correctly.
Home Exercise Program:
At this stage, we needed to improve the robustness of the craniovertebral stabilizers as her motor control strategy was not restored by just correcting the alignment of the cranial region. We began Stage 2 motor control retraining to improve the capacity of her cranio-vertebral stabilizers. I asked Mrs. B to place two targets on the wall at home approximately arm’s length apart. Mrs. B’s task was to first align cranium with “space behind right ear” cue and then spend 30 seconds jumping gaze between the two targets. Initially, she needed tactile feedback of fingers on her mastoid processes to keep cranium steady and to note when her strategy started to become suboptimal. She was asked to increase the duration up to one minute gradually as her endurance improved; stopping if her symptoms returned or she felt either of her mastoid processes move under her fingers.
Further Follow-up Sessions
Mrs. B’s weekly treatment gradually transitioned from an emphasis on releasing the cranium to controlling her new alignment as we added sensorimotor retraining exercises common to post concussive rehabilitation. We also worked on incorporating cranial alignment into various yoga positions during her teaching.
Her progress was not strictly linear; she had good and bad days depending on how much she pushed herself or what her work schedule was like. She also suffered a shoulder injury during a yoga practice which changed our focus for a few sessions. Her dizziness symptoms gradually reduced in both intensity and frequency as her new strategy of cranial control (cranium and OA and AA joints) became more automatic and her sensorimotor systems became more robust.
Her initial significant change in symptom presentation was likely due to draining the dural venous system inside her cranium. As I mentioned, the cranial nerve supply to the eyes has intra- and interdural segments which are tensioned by the venous backflow in the sinuses which pulls on the cerebellar tentorium. Her lingering symptoms of frontal bone headaches, “yucky” feeling and recall issues gradually improved as she worked to create a new habitual strategy to control her cranium, keeping the jugular foramen patent and prevent the backflow of pressure from reoccurring.
Diane’s comment:
Excellent report Courtney.
References
- Slater et al 2019 Sit up Straight. Time to Re-evaluate. JOSPT 49:8 p 562
- Giza, C. C., & Hovda, D. A. (2014). The new neurometabolic cascade of concussion. Neurosurgery, 75(suppl_4), S24-S33.
- Haider, M. N., Leddy, J. J., Hinds, A. L., Aronoff, N., Rein, D., Poulsen, D., & Willer, B. S. (2018). Intracranial pressure changes after mild traumatic brain injury: a systematic review. Brain injury, 32(7), 809-815.
- Signoretti, S., Lazzarino, G., Tavazzi, B., & Vagnozzi, R. (2011). The pathophysiology of concussion. Pm&r, 3(10), S359-S368.
- Curé, J. K., Van Tassel, P., & Smith, M. T. (1994, December). Normal and variant anatomy of the dural venous sinuses. In Seminars in ultrasound, CT, and MR (Vol. 15, No. 6, pp. 499-519).
- Liu, J. K., Gupta, G., Christiano, L. D., & Fukushima, T. (2012). Surgical Management of Tumors of the Jugular Foramen. In Schmidek and Sweet Operative Neurosurgical Techniques: Indications, Methods, and Results: Sixth Edition (Vol. 1, pp. 529-545). Elsevier Inc.. https://doi.org/10.1016/B978-1-4160-6839-6.10044-9
- Iaconetta, G., Fusco, M., Cavallo, L. M., Cappabianca, P., Samii, M., & Tschabitscher, M. (2007). The abducens nerve: microanatomic and endoscopic study. Operative Neurosurgery, 61(suppl_3), ONS-7.
- Iaconetta, G., de Notaris, M., Cavallo, L. M., Benet, A., Enseñat, J., Samii, M., … & Cappabianca, P. (2010). The oculomotor nerve: microanatomical and endoscopic study. Neurosurgery, 66(3), 593-601
- Rai, R., Iwanaga, J., Shokouhi, G., Oskouian, R. J., & Tubbs, R. S. (2018). The tentorium cerebelli: a comprehensive review including its anatomy, embryology, and surgical techniques. Cureus, 10(7).
- Grossman, E. J., Jensen, J. H., Babb, J. S., Chen, Q., Tabesh, A., Fieremans, E., Xia, D., Inglese, M., & Grossman, R. I. (2013). Cognitive impairment in mild traumatic brain injury: a longitudinal diffusional kurtosis and perfusion imaging study. American journal of neuroradiology, 34(5), 951–S3. https://doi.org/10.3174/ajnr.A3358
Skills Demonstration
Case Study Author
Clinical Mentorship in the Integrated Systems Model
Join Diane, and her team of highly skilled assistants, on this mentorship journey and immerse yourself in a series of education opportunities that will improve your clinical efficacy for treating the whole person using the updated Integrated Systems Model.
We will come together for 3 sessions of 4 (4.5) days over a period of 6-8 months with lots of practical/clinical time to focus on acquiring the skills and clinical reasoning to put the ISM model into practice. Hours of online lecture and reading material and 12 hours of in-person lecture are...
More Info